Dwivraniya Chikitsa
Chikitsa Sthana Chapter 25. Management of two types of Vrana (ulcers)
| Section/Chapter | Chikitsa Sthana Chapter 25 |
|---|---|
| Preceding Chapter | Madatyaya Chikitsa |
| Succeeding Chapter | Trimarmiya Chikitsa |
| Other Sections | Sutra Sthana, Nidana Sthana, Vimana Sthana, Sharira Sthana, Indriya Sthana, Kalpa Sthana, Siddhi Sthana |
| Translator and commentator | Singh L., Sharma A., Dudhamal T.S. |
| Reviewer | Dudhamal T.S. |
| Editors | Dudhamal T.S., Deole Y.S., Basisht G. |
| Year of publication | 2020 |
| Publisher | Charak Samhita Research, Training and Skill Development Centre |
| DOI | 10.47468/CSNE.2020.e01.s06.026 |
Abstract
Vrana (ulcers) are of two types, nija vrana (endogenous ulcers) and agantuka vrana (exogenous ulcers). This classification is based on etiology and mode of treatments. Endogenous ulcers are caused by vitiation of vata etc. dosha from initial stage while exogenous ulcers are caused initially by various types of trauma and later dosha vitiation occurs. Complications of ulcers like visarpa (erysipelas), sirastambha (constricted vessels), jwara (fever) etc. have been described. Importance of bloodletting is described during the stage of vrana shopha (i.e.inflammatory phase), alleviation of impure blood from body reduces toxic chemicals and pacifies dosha. Description of fracture, its complications and management is elaborated. Dahakarma (cauterization) causes constriction of blood vessels to prevent bleeding from ulcer. Application of alkaline substances (kshara) on ulcer can be done along with surgical intervention and cauterization. Prognosis of ulcer can be described on the basis of type of ulcer and its various locations.
Keywords: Vrana (ulcer), trividha pariksha, bloodletting, dahakarma (cauterization), shodhanakarma (cleansing of ulcer), ropankarma (healing of ulcer), wound management, non healing ulcers.
Introduction
The term vrana literally means destruction or rupture or discontinuation of body tissues. This chapter gives comprehensive information about endogenous and exogenous ulcers. Trividha pariksha or three different ways of examination of ulcer is done by darshana (inspection), prashna (interrogation) and sparshana (palpation). Inspection i.e. visual examination deals with general examination (whole body) and local examination (specific part or organ) to make proper diagnosis. The etiological factors, nature of pain, ability to get used to food (satmya/asatmya), drugs, status of digestive power etc are examined by interrogation. Palpation is the mode of direct examination done by palpating the margin, size, depth, temperature, stiffness or hardness etc. Prognosis of ulcer is determined by its location eg. skin (tvaka), blood vessels (shira), muscle tissue (mamsa dhatu), fatty tissue (meda dhatu), bone (asthi dhatu), ligament (snayu), vital organs (marma)[1],visceras of chest and abdomen (antarashraya)[2] [ Cha. Sa. Sharira Sthana 7/10 ]
Various complications of ulcers like visarpa (erysipelas), pakshaghata (hemiplegia), shirastambha (constricted vessels), jwara (fever) etc. are described. Sloughing of ligaments and vessels, deep seated appearance of maggots, fracture of bone near the ulcer, presence of foreign body in the ulcer etc hamper the healing process. Treatment of nija vrana (endogenous ulcer)[3] is different from agantuja vrana (exogenous ulcer) because endogenous ulcers are caused by vitiation of vatadi doshaja, and exogenous ulcers are initially caused by various type of trauma such as vadha (stab injury etc.), bandha (excessive tying), prapatana (injury due to fall), injury due to teeth and nail etc. But later on in exogenous ulcers also involvement of dosha takes place and then treatment should be adopted as nija vrana (endogenous ulcer). In endogenous ulcers, shodhana therapy should be adopted by vamana (emesis), virechana (purgation) and basti (medicated enema) and blood letting for removal of doshaja (toxic materials) from body. [ Cha. Sa. Sutra Sthana 16/17 ] and agnikarma. Agnikarma has ushna guna (hot property) which is opposite to vata and kapha. Due to heat, vasodilation leads to alleviation of srotorodha resulting in proper vascularity to organ or part. In exogenous ulcers, local treatment with use of kshara (alkaline substances), surgical intervention and cauterization is recommended.
Sanskrit Text, Transliteration and English Translation
अथातो द्विव्रणीयचिकित्सितं व्याख्यास्यामः ||१||
इति ह स्माह भगवानात्रेयः ||२||
athātō dvivraṇīyacikitsitaṁ vyākhyāsyāmaḥ||1||
iti ha smāha bhagavānātrēyaḥ||2||
athAto dvivraNIyacikitsitaM vyAkhyAsyAmaH ||1||
iti ha smAha bhagavAnAtreyaH ||2||
Now we shall expound the chapter "Dwivraniya chikitsa" (Management of two types of ulcers).Thus said Lord Atreya.[1-2]
Query by Agnivesha
परावरज्ञमात्रेयं गतमानमदव्यथम् |
अग्निवेशो गुरुं काले विनयादिदमब्रवीत् ||३||
भगवन्! पूर्वमुद्दिष्टौ द्वौ व्रणौ रोगसङ्ग्रहे |
तयोर्लिङ्गं चिकित्सां च वक्तुमर्हसि शर्मद! ||४||
parāvarajñamātrēyaṁ gatamānamadavyatham|
agnivēśō guruṁ kālē vinayādidamabravīt||3||
bhagavan! pūrvamuddiṣṭau dvau vraṇau rōgasaṅgrahē|
tayōrliṅgaṁ cikitsāṁ ca vaktumarhasi śarmada!||4||
parAvaraj~jamAtreyaM gatamAnamadavyatham |
agnivesho guruM kAle vinayAdidamabravIt ||3||
bhagavan! pUrvamuddiShTau dvau vraNau rogasa~ggrahe |
tayorli~ggaM cikitsAM ca vaktumarhasi sharmada! ||4||
Agnivesha, in opportune moment, respectfully submitted to his teacher Atreya, knower of the best and the worst and devoid of conceit, ego and suffering –“ O Lord ! Two types of ulcers have been mentioned earlier under enumeration of disorders; kindly describe their symptoms and treatment O conferer of happiness!”[3-4]
Classification and etiology of vrana
इत्यग्निवेशस्य वचो निशम्य गुरुरब्रवीत् |
यौ व्रणौ पूर्वमुद्दिष्टौ निजश्चागन्तुरेव च ||५||
श्रूयतां विधिवत् सौम्य! तयोर्लिङ्गं च [१] भेषजम् |
निजः शरीरदोषोत्थ आगन्तुर्बाह्यहेतुजः ||६||
वधबन्धप्रपतनाद्दंष्ट्रादन्तनखक्षतात् |
आगन्तवो व्रणास्तद्वद्विषस्पर्शाग्निशस्त्रजाः ||७||
मन्त्रागदप्रलेपाद्यैर्भेषजैर्हेतुभिश्च ते |
लिङ्गैकदेशैर्निर्दिष्टा विपरीता निजैर्व्रणैः [२] ||८||
ityagnivēśasya vacō niśamya gururabravīt|
yau vraṇau pūrvamuddiṣṭau nijaścāganturēva ca||5||
śrūyatāṁ vidhivat saumya! tayōrliṅgaṁ ca [1] bhēṣajam|
nijaḥ śarīradōṣōttha āganturbāhyahētujaḥ||6||
vadhabandhaāddprapatanaṁṣṭrādantanakhakṣatāt|
āgantavō vraṇāstadvadviṣasparśāgniśastrajāḥ||7||
mantrāgadapralēpādyairbhēṣajairhētubhiśca tē|
liṅgaikadēśairnirdiṣṭā viparītā nijairvraṇaiḥ [2] ||8||
ityagniveshasya vaco nishamya gururabravIt |
yau vraNau pUrvamuddiShTau nijashcAgantureva ca ||5||
shrUyatAM vidhivat saumya! tayorli~ggaM ca [1] bheShajam |
nijaH sharIradoShottha AganturbAhyahetujaH ||6||
vadhabandhaprapatanAddaMShTrAdantanakhakShatAt |
Agantavo vraNAstadvadviShasparshAgnishastrajAH ||7||
mantrAgadapralepAdyairbheShajairhetubhishca te |
li~ggaikadeshairnirdiShTA viparItA nijairvraNaiH [2] ||8||
After listening the request of Agnivesa the teacher said – ‘O gentle! Listen about the symptoms and treatment of the two types of vrana (ulcers) , endogenous ulcer and exogenous ulcer, as mentioned earlier.The endogenous ulcers occur from the bodily dosha, whereas the exogenous ulcers are caused by external causative factors. Exogenous ulcer are caused by blowing, binding, falling down, injury with fangs, teeth or nails as well as due to poisonous contact, fire and weapons etc. Exogenous ulcers are different from the endogenous ones in respect of treatment with mantra (incantations), anti-poisonous pastes for external application etc. While endogenous ulcer bears opposite characteristic features in respect of etiology, sign symptoms and treatment. [5-8]
Importance of dosha dominance in treatment
व्रणानां निजहेतूनामागन्तूनामशाम्यताम् |
कुर्याद्दोषबलापेक्षी निजानामौषधं यथा ||९||
vraṇānāṁ nijahētūnāmāgantūnāmaśāmyatām|
kuryāddōṣabalāpēkṣī nijānāmauṣadhaṁ yathā||9||
vraNAnAM nijahetUnAmAgantUnAmashAmyatAm |
kuryAddoShabalApekShI nijAnAmauShadhaM yathA ||9||
Exogenous ulcers not being pacified and having endogenous causative factors should be treated as endogenous ulcers according to predominance of dosha.[9]
Endogenous ulcers
यथास्वैर्हेतुभिर्दुष्टा वातपित्तकफा नृणाम् |
बहिर्मार्गं समाश्रित्य जनयन्ति निजान् व्रणान् ||१०||
yathāsvairhētubhirduṣṭā vātapittakaphā nr̥ṇām|
bahirmārgaṁ samāśritya janayanti nijān vraṇān||10||
yathAsvairhetubhirduShTA vAtapittakaphA nRuNAm |
bahirmArgaM samAshritya janayanti nijAn vraNAn ||10||
Vata, pitta and kapha are vitiated by their respective causes get lodged in external passage and thus produce endogenous ulcers. [10]
Dosha dominant vrana and their treatment
Vata dominant vrana and treatment
स्तब्धः कठिनसंस्पर्शो मन्दस्रावोऽतितीव्ररुक् [१] |
तुद्यते स्फुरति श्यावो व्रणो मारुतसम्भवः ||११||
सम्पूरणैः स्नेहपानैः स्निग्धैः स्वेदोपनाहनैः |
प्रदेहैः परिषेकैश्च वातव्रणमुपाचरेत् ||१२||
stabdhaḥ kaṭhinasaṁsparśō mandasrāvō'titīvraruk [1] |
tudyatē sphurati śyāvō vraṇō mārutasambhavaḥ||11||
sampūraṇaiḥ snēhapānaiḥ snigdhaiḥ svēdōpanāhanaiḥ|
pradēhaiḥ pariṣēkaiśca vātavraṇamupācarēt||12||
stabdhaH kaThinasaMsparsho mandasrAvo~atitIvraruk [1] |
tudyate sphurati shyAvo vraNo mArutasambhavaH ||11||
sampUraNaiH snehapAnaiH snigdhaiH svedopanAhanaiH |
pradehaiH pariShekaishca vAtavraNamupAcaret ||12||
The ulcer caused by vata is stiff, hard to touch, with scanty exudation, excruciating and pricking pain with throbbing and blackish discoloration. Vatika ulcer should be treated with sampurana (filling of ulcer cavity), intake of unctuous substances (oleation therapy), unctuous fomentation and poultices, ointments and sprinklings.[11-12]
Pitta dominant vrana and treatment
तृष्णामोहज्वरस्वे(क्ले)ददाहदुष्ट्यवदारणैः |
व्रणं पित्तकृतं विद्याद्गन्धैः स्रावैश्च पूतिकैः ||१३||
शीतलैर्मधुरैस्तिक्तैः प्रदेहपरिषेचनैः |
सर्पिष्पानैर्विरेकैश्च पैत्तिकं शमयेद्व्रणम् ||१४||
tr̥ṣṇāmōhajvarasvē(klē)dadāhaduṣṭyavadāraṇaiḥ|
vraṇaṁ pittakr̥taṁ vidyādgandhaiḥ srāvaiśca pūtikaiḥ||13||
śītalairmadhuraistiktaiḥ [2] pradēhapariṣēcanaiḥ|
sarpiṣpānairvirēkaiśca paittikaṁ śamayēdvraṇam||14||
tRuShNAmohajvarasve(kle)dadAhaduShTyavadAraNaiH |
vraNaM pittakRutaM vidyAdgandhaiH srAvaishca pUtikaiH ||13||
shItalairmadhuraistiktaiH [2] pradehapariShecanaiH |
sarpiShpAnairvirekaishca paittikaM shamayedvraNam ||14||
Pittaja ulcer is known from thirst, unconsciousness, fever, sweating, burning sensation, impurity, tearing and foul smell with discharge of pus from ulcer. One should pacify the pittaja ulcer by anointing and sprinkling with cold, intake of sweet and bitter drugs, intake of ghee and purgation. [13-14]
Kapha dominant vrana and treatment
बहुपिच्छो गुरुः स्निग्धः स्तिमितो मन्दवेदनः |
पाण्डुवर्णोऽल्पसङ्क्लेदश्चिरकारी कफव्रणः ||१५||
कषायकटुरूक्षोष्णैः प्रदेहपरिषेचनैः |
कफव्रणं प्रशमयेत्तथा लङ्घनपाचनैः [३] ||१६||
bahupicchō guruḥ snigdhaḥ stimitō mandavēdanaḥ|
pāṇḍuvarṇō'lpasaṅklēdaścirakārī kaphavraṇaḥ||15||
kaṣāyakaṭurūkṣōṣṇaiḥ pradēhapariṣēcanaiḥ|
kaphavraṇaṁ praśamayēttathā laṅghanapācanaiḥ [3] ||16||
bahupiccho guruH snigdhaH stimito mandavedanaH |
pANDuvarNo~alpasa~gkledashcirakArI kaphavraNaH ||15||
kaShAyakaTurUkShoShNaiH pradehapariShecanaiH |
kaphavraNaM prashamayettathA la~gghanapAcanaiH [3] ||16||
Kaphaja ulcer has much sliminess, heavyness, unctuousness, numbness, with mild pain, paleness in color, little slough and prolonged healing. Kaphaja ulcer is treated with anointing and sprinkling with astringent, pungent, dry and hot drugs as well as fasting and digestive measures.[15-16]
तौ द्वौ नानात्वभेदेन निरुक्ता विंशतिर्व्रणाः |
तेषां परीक्षा त्रिविधा, प्रदुष्टा द्वादश स्मृताः ||१७||
स्थानान्यष्टौ तथा गन्धाः, परिस्रावाश्चतुर्दश |
षोडशोपद्रवा दोषाश्चत्वारो विंशतिस्तथा ||१८||
तथा चोपक्रमाः सिद्धाः षट्त्रिंशत् समुदाहृताः |
विभज्यमानाञ्छृणु [१] मे सर्वानेतान् यथेरितान् ||१९||
tau dvau nānātvabhēdēna niruktā viṁśatirvraṇāḥ|
tēṣāṁ parīkṣā trividhā, praduṣṭā dvādaśa smr̥tāḥ||17||
sthānānyaṣṭau tathā gandhāḥ, parisrāvāścaturdaśa|
ṣōḍaśōpadravā dōṣāścatvārō viṁśatistathā||18||
tathā cōpakramāḥ siddhāḥ ṣaṭtriṁśat samudāhr̥tāḥ|
vibhajyamānāñchr̥ṇu [1] mē sarvānētān yathēritān||19||
tau dvau nAnAtvabhedena niruktA viMshatirvraNAH |
teShAM parIkShA trividhA, praduShTA dvAdasha smRutAH ||17||
sthAnAnyaShTau tathA gandhAH, parisrAvAshcaturdasha |
ShoDashopadravA doShAshcatvAro viMshatistathA ||18||
tathA copakramAH siddhAH ShaTtriMshat samudAhRutAH |
vibhajyamAnA~jchRuNu [1] me sarvAnetAn yatheritAn ||19||
Above two types of ulcers are further divided into twenty types on the basis of distinctive features. Their examination can be done by three ways, signs of excess vitiation at site of ulcers are of twelve types, eight locations, fourteen types of discharges, sixteen complications, twenty four defects and thirty six therapeutic measures. Now listen about these in details. [17-19]
Twenty types of ulcers
कृत्योत्कृत्यस्तथा [१] दुष्टोऽदुष्टो मर्मस्थितो न च |
संवृतो दारुणः स्रावी सविषो विषमस्थितः ||२०||
उत्सङ्ग्युत्सन्न एषां च व्रणान् विद्याद्विपर्ययात् |
इति नानात्वभेदेन निरुक्ता [२] विंशतिर्व्रणाः ||२१||
kr̥tyōtkr̥tyastathā [1] duṣṭō'duṣṭō marmasthitō na ca|
saṁvr̥tō dāruṇaḥ srāvī saviṣō viṣamasthitaḥ||20||
utsaṅgyutsanna ēṣāṁ ca vraṇān vidyādviparyayāt|
iti nānātvabhēdēna niruktā [2] viṁśatirvraṇāḥ||21||
kRutyotkRutyastathA [1] duShTo~aduShTo marmasthito na ca |
saMvRuto dAruNaH srAvI saviSho viShamasthitaH ||20||
utsa~ggyutsanna eShAM ca vraNAn vidyAdviparyayAt |
iti nAnAtvabhedena niruktA [2] viMshatirvraNAH ||21||
Curable (can be treated with surgical intervention), incurable; infected, non-infected; situated in vital parts, not situated in vital parts; closed, open; hard, soft; discharging, non-discharging; poisonous, non-poisonous; unevenly located, evenly located; pouched, un-pouched; elevated, depressed – these are the twenty types of ulcers according to various distinguishing features.[20-21]
Three fold examination
दर्शनप्रश्नसंस्पर्शैः परीक्षा त्रिविधा स्मृता |
वयोवर्णशरीराणामिन्द्रियाणां च दर्शनात् ||२२||
हेत्वर्तिसात्म्याग्निबलं परीक्ष्यं वचनाद्बुधैः |
स्पर्शान्मार्दवशैत्ये च परीक्ष्ये सविपर्यये ||२३||
darśanapraśnasaṁsparśaiḥ parīkṣā trividhā smr̥tā|
vayōvarṇaśarīrāṇāmindriyāṇāṁ ca darśanāt||22||
hētvartisātmyāgnibalaṁ parīkṣyaṁ vacanādbudhaiḥ|
sparśānmārdavaśaityē ca parīkṣyē saviparyayē||23||
darshanaprashnasaMsparshaiH parIkShA trividhA smRutA |
vayovarNasharIrANAmindriyANAM ca darshanAt ||22||
hetvartisAtmyAgnibalaM parIkShyaM vacanAdbudhaiH |
sparshAnmArdavashaitye ca parIkShye saviparyaye ||23||
Examination of ulcer can be performed by three methods e.g. by inspection, interrogation and palpation.
Age, complexion and color, body parts and sense organs are examined by inspection. Etiology, nature of pain, suitability and power of digestion should be known by patient’s statement. By palpation softness and coldness are known with their contraries. [22-23]
Twelve types of ulcers
श्वेतोऽवसन्नवर्त्माऽतिस्थूलवर्त्माऽतिपिञ्जरः [१] |
नीलःश्यावोऽतिपिडको रक्तः कृष्णोऽतिपूतिकः ||२४||
रोप्यः कुम्भीमुखश्चेति प्रदुष्टा द्वादश व्रणाः |
चतुर्विंशतिरुद्दिष्टा [२] दोषाः कल्पान्तरेण वै ||२५||
śvētō'vasannavartmā'tisthūlavartmā'tipiñjaraḥ [1] |
nīlaḥśyāvō'tipiḍakō raktaḥ kr̥ṣṇō'tipūtikaḥ||24||
rōpyaḥ kumbhīmukhaścēti praduṣṭā dvādaśa vraṇāḥ|
caturviṁśatiruddiṣṭā [2] dōṣāḥ kalpāntarēṇa vai||25||
shveto~avasannavartmA~atisthUlavartmA~atipi~jjaraH [1] |
nIlaHshyAvo~atipiDako raktaH kRuShNo~atipUtikaH ||24||
ropyaH kumbhImukhashceti praduShTA dvAdasha vraNAH |
caturviMshatiruddiShTA [2] doShAH kalpAntareNa vai ||25||
White, with depressed margins, very thick margins, much greyish (pinjara), blue, blackish, surrounded with numerous boils, red, black, very fetid odor, non- healing nature and bottle-necked (narrow opening) these are twelve types of defective (dushta) ulcers.[24-25]
Sites of vitiation
त्वक्सिरामांसमेदोऽस्थिस्नायुमर्मान्तराश्रयाः |
व्रणस्थानानि निर्दिष्टान्यष्टावेतानि सङ्ग्रहे ||२६||
tvaksirāmāṁsamēdō'sthisnāyumarmāntarāśrayāḥ|
vraṇasthānāni nirdiṣṭānyaṣṭāvētāni saṅgrahē||26||
tvaksirAmAMsamedo~asthisnAyumarmAntarAshrayAH |
vraNasthAnAni nirdiShTAnyaShTAvetAni sa~ggrahe ||26||
In the treatise, eight locations of wounds have been mentioned such as skin, blood vessels, flesh, fat, bone, ligament, vital parts and viscera.[26]
Specific odors of vrana
सर्पिस्तैलवसापूयरक्तश्यावाम्लपूतिकाः |
व्रणानां व्रणगन्धज्ञैरष्टौ गन्धाः प्रकीर्तिताः ||२७||
sarpistailavasāpūyaraktaśyāvāmlapūtikāḥ|
vraṇānāṁ vraṇagandhajñairaṣṭau gandhāḥ prakīrtitāḥ||27||
sarpistailavasApUyaraktashyAvAmlapUtikAH |
vraNAnAM vraNagandhaj~jairaShTau gandhAH prakIrtitAH ||27||
Eight types of wound odors have been defined by the experts like ghee, oil, muscle-fat, pus, blood, and cadaver, sour and fetid.[27]
Fourteen types of discharges and sixteen complications
लसीकाजलपूयासृग्घारिद्रारुणपिञ्जराः |
कषायनीलहरितस्निग्धरूक्षसितासिताः ||२८||
इति रूपैः समुद्दिष्टा व्रणस्रावाश्चतुर्दश |
विसर्पः पक्षघातश्च सिरास्तम्भोऽपतानकः ||२९||
मोहोन्मादव्रणरुजो ज्वरस्तृष्णा हनुग्रहः |
कासश्छर्दिरतीसारो हिक्का श्वासः सवेपथुः ||३०||
षोडशोपद्रवाः प्रोक्ता व्रणानां व्रणचिन्तकैः |३१|
lasīkājalapūyāsr̥gghāridrāruṇapiñjarāḥ|
kaṣāyanīlaharitasnigdharūkṣasitāsitāḥ||28||
iti rūpaiḥ samuddiṣṭā vraṇasrāvāścaturdaśa|
visarpaḥ pakṣaghātaśca sirāstambhō'patānakaḥ||29||
mōhōnmādavraṇarujō jvarastr̥ṣṇā hanugrahaḥ|
kāsaśchardiratīsārō hikkā śvāsaḥ savēpathuḥ||30||
ṣōḍaśōpadravāḥ prōktā vraṇānāṁ vraṇacintakaiḥ|31|
lasIkAjalapUyAsRugghAridrAruNapi~jjarAH |
kaShAyanIlaharitasnigdharUkShasitAsitAH ||28||
iti rUpaiH samuddiShTA vraNasrAvAshcaturdasha |
visarpaH pakShaghAtashca sirAstambho~apatAnakaH ||29||
mohonmAdavraNarujo jvarastRuShNA hanugrahaH |
kAsashchardiratIsAro hikkA shvAsaH savepathuH ||30||
ShoDashopadravAH proktA vraNAnAM vraNacintakaiH |31|
Discharges from ulcers are of fourteen types in appearance such as lasika (like lymph), water, pus, blood, color of exudation as yellow, reddish, brownish, ochre-colored, blue, green, unctuous, rough, white and black.
The experts have mentioned sixteen complications of wounds such as erysipelas, paralysis, occlusion in blood vessels, tetanus, and mental confusion, and insanity, pain in wound, fever, thirst, lockjaw, cough, vomiting, diarrhea, hiccups, dyspnea and trembling.[28-31]
Causes of non-healing ulcers
स्नायुक्लेदात्सिराक्लेदाद्गाम्भीर्यात्कृमिभक्षणात् [१] ||३१||
अस्थिभेदात् सशल्यत्वात् सविषत्वाच्च [२] सर्पणात् |
नखकाष्ठप्रभेदाच्च चर्मलोमातिघट्टनात् [३] ||३२||
मिथ्याबन्धादति स्नेहादतिभैषज्यकर्षणात् |
अजीर्णादतिभुक्ताच्च विरुद्धासात्म्यभोजनात् ||३३||
शोकात् क्रोधाद्दिवास्वप्नाद्व्यायामान्मैथुनात्तथा |
व्रणा न प्रशमं यान्ति निष्क्रियत्वाच्च देहिनाम् ||३४||
परिस्रावाच्च गन्धाच्च दोषाच्चोपद्रवैः सह |
व्रणानां बहुदोषाणां कृच्छ्रत्वं चोपजायते ||३५||
snāyuklēdātsirāklēdādgāmbhīryātkr̥mibhakṣaṇāt [1] ||31||
asthibhēdāt saśalyatvāt saviṣatvācca [2] sarpaṇāt|
nakhakāṣṭhaprabhēdācca carmalōmātighaṭṭanāt [3] ||32||
mithyābandhādati snēhādatibhaiṣajyakarṣaṇāt|
ajīrṇādatibhuktācca viruddhāsātmyabhōjanāt||33||
śōkāt krōdhāddivāsvapnādvyāyāmānmaithunāttathā|
vraṇā na praśamaṁ yānti niṣkriyatvācca dēhinām||34||
parisrāvācca gandhācca dōṣāccōpadravaiḥ saha|
vraṇānāṁ bahudōṣāṇāṁ kr̥cchratvaṁ cōpajāyatē||35||
snAyukledAtsirAkledAdgAmbhIryAtkRumibhakShaNAt [1] ||31||
asthibhedAt sashalyatvAt saviShatvAcca [2] sarpaNAt |
nakhakAShThaprabhedAcca carmalomAtighaTTanAt [3] ||32||
mithyAbandhAdati snehAdatibhaiShajyakarShaNAt |
ajIrNAdatibhuktAcca viruddhAsAtmyabhojanAt ||33||
shokAt krodhAddivAsvapnAdvyAyAmAnmaithunAttathA |
vraNA na prashamaM yAnti niShkriyatvAcca dehinAm ||34||
parisrAvAcca gandhAcca doShAccopadravaiH saha |
vraNAnAM bahudoShANAM kRucchratvaM copajAyate ||35||
Defects are known to be twenty four according to etiological factors which are as follows: moistening of ligaments, excess of fluid in blood vessels, deepness, eaten by maggots, cracking of bones, presence of foreign body, presence of toxins, spreading, excessive tearing with nails or wooden piece, friction of skin, friction of body hair, faulty bandage, over-application of uncting substance, excessive emaciation due to over dose, indigestion, over-eating, intake of incompatible food items, unsuitable food, grief, anger, day-sleep, physical exercise, sexual intercourse and inactivity.These factors lead to delay in the healing process. Ulcers having much impurity become difficult to be cured due to presence of excessive discharges, odors, defects and complications.[31-35]
Factors affecting prognosis
त्वङ्मांसजः सुखे देशे तरुणस्यानुपद्रवः |
धीमतोऽभिनवः काले सुखसाध्यः स्मृतो व्रणः ||३६||
गुणैरन्यतमैर्हीनस्ततः कृच्छ्रो व्रणः स्मृतः |
सर्वैर्विहीनो विज्ञेयस्त्वसाध्यो निरुपक्रमः [१] ||३७||
tvaṅmāṁsajaḥ sukhē dēśē taruṇasyānupadravaḥ|
dhīmatō'bhinavaḥ kālē sukhasādhyaḥ smr̥tō vraṇaḥ||36||
guṇairanyatamairhīnastataḥ kr̥cchrō vraṇaḥ smr̥taḥ|
sarvairvihīnō vijñēyastvasādhyō nirupakramaḥ [1] ||37||
tva~gmAMsajaH sukhe deshe taruNasyAnupadravaH |
dhImato~abhinavaH kAle sukhasAdhyaH smRuto vraNaH ||36||
guNairanyatamairhInastataH kRucchro vraNaH smRutaH |
sarvairvihIno vij~jeyastvasAdhyo nirupakramaH [1] ||37||
Wound is easily curable if it is located in skin and muscles, easy places, youthful age, without complication, in a wise patient and of recent origin. If it is devoid of some of these qualities it is curable with difficulty and when it is devoid of all the qualities it is incurable and thus not to be treated.[36-37]
Principles of management
व्रणानामादितः कार्यं यथासन्नं विशोधनम् |
ऊर्ध्वभागैरधोभागैः शस्त्रैर्बस्तिभिरेव च ||३८||
सद्यः शुद्धशरीराणां प्रशमं यान्ति हि व्रणाः |३९|
vraṇānāmāditaḥ kāryaṁ yathāsannaṁ viśōdhanam|
ūrdhvabhāgairadhōbhāgaiḥ śastrairbastibhirēva ca||38||
sadyaḥ śuddhaśarīrāṇāṁ praśamaṁ yānti hi vraṇāḥ|39|
vraNAnAmAditaH kAryaM yathAsannaM vishodhanam |
UrdhvabhAgairadhobhAgaiH shastrairbastibhireva ca ||38||
sadyaH shuddhasharIrANAM prashamaM yAnti hi vraNAH |39|
In cases of wound, first of all, purification with therapeutic emesis, purgation, shastra karma (surgical intervention) and basti (medicated enema) should be done after assessment of condition because the wounds get healed quickly in those with cleansed body.[38-39]
Procedures for management of ulcers
यथाक्रममतश्चोर्ध्वं शृणु सर्वानुपक्रमान् ||३९||
शोफघ्नं षड्विधं चैव शस्त्रकर्मावपीडनम् |
निर्वापणं ससन्धानं स्वेदः शमनमेषणम् ||४०||
शोधनौ रोपणीयौ च कषायौ सप्रलेपनौ |
द्वे तैले तद्गुणे [१] पत्रं छादने द्वे च बन्धने ||४१||
भोज्यमुत्सादनं दाहो द्विविधः सावसादनः |
काठिन्यमार्दवकरे धूपनालेपने शुभे ||४२||
व्रणावचूर्णनं वर्ण्यं रोपणं लोमरोहणम् |
इति षट्त्रिंशदुद्दिष्टा व्रणानां समुपक्रमाः ||४३||
yathākramamataścōrdhvaṁ śr̥ṇu sarvānupakramān||39||
śōphaghnaṁ ṣaḍvidhaṁ caiva śastrakarmāvapīḍanam|
nirvāpaṇaṁ sasandhānaṁ svēdaḥ śamanamēṣaṇam||40||
śōdhanau rōpaṇīyau ca kaṣāyau sapralēpanau|
dvē tailē tadguṇē [1] patraṁ chādanē dvē ca bandhanē||41||
bhōjyamutsādanaṁ dāhō dvividhaḥ sāvasādanaḥ|
kāṭhinyamārdavakarē dhūpanālēpanē śubhē||42||
vraṇāvacūrṇanaṁ varṇyaṁ rōpaṇaṁ lōmarōhaṇam|
iti ṣaṭtriṁśaduddiṣṭā vraṇānāṁ samupakramāḥ||43||
yathAkramamatashcordhvaM shRuNu sarvAnupakramAn ||39||
shophaghnaM ShaDvidhaM caiva shastrakarmAvapIDanam |
nirvApaNaM sasandhAnaM svedaH shamanameShaNam ||40||
shodhanau ropaNIyau ca kaShAyau sapralepanau |
dve taile tadguNe [1] patraM chAdane dve ca bandhane ||41||
bhojyamutsAdanaM dAho dvividhaH sAvasAdanaH |
kAThinyamArdavakare dhUpanAlepane shubhe ||42||
vraNAvacUrNanaM varNyaM ropaNaM lomarohaNam |
iti ShaTtriMshaduddiShTA vraNAnAM samupakramAH ||43||
Hereafter listen about all the measures of treatment in order such as – measures for pacification of swelling, six types of surgical operations, pressing, cooling?, uniting, fomentation, pacification, probing, cleansing, healing, cleaning paste, healing paste, cleaning oil, healing oil, two types of covering with leaf, two types of bandaging, diet, elevation, two types of cauterization, depression, hardening fumigation, softening fumigation, hardening paste, softening paste, powdering, colorization, healing, repilatory- these are the thirty six measures of treatment of wounds.[39-43]
Guidelines for management of ulcers
पूर्वरूपं भिषग्बुद्ध्वा व्रणानां शोफमादितः |
रक्तावसेचनं कुर्यादजातव्रणशान्तये ||४४||
शोधयेद्बहुदोषांस्तु स्वल्पदोषान् विलङ्घयेत् |
पूर्वं कषायसर्पिर्भिर्जयेद्वा मारुतोत्तरान् ||४५||
न्यग्रोधोदुम्बराश्वत्थप्लक्षवेतसवल्कलैः |
ससर्पिष्कैः प्रलेपः स्याच्छोफनिर्वापणः परम् ||४६||
विजया मधुकं वीरा बिसग्रन्थिः शतावरी |
नीलोत्पलं नागपुष्पं प्रदेहः स्यात् सचन्दनः ||४७||
सक्तवो मधुकं सर्पिः प्रदेहः स्यात् सशर्करः |
अविदाहीनि चान्नानि शोफे भेषजमुत्तमम् ||४८||
pūrvarūpaṁ bhiṣagbuddhvā vraṇānāṁ śōphamāditaḥ|
raktāvasēcanaṁ kuryādajātavraṇaśāntayē||44||
śōdhayēdbahudōṣāṁstu svalpadōṣān vilaṅghayēt|
pūrvaṁ kaṣāyasarpirbhirjayēdvā mārutōttarān||45||
nyagrōdhōdumbarāśvatthaplakṣavētasavalkalaiḥ|
sasarpiṣkaiḥ pralēpaḥ syācchōphanirvāpaṇaḥ param||46||
vijayā madhukaṁ vīrā bisagranthiḥ śatāvarī|
nīlōtpalaṁ nāgapuṣpaṁ pradēhaḥ syāt sacandanaḥ||47||
saktavō madhukaṁ sarpiḥ pradēhaḥ syāt saśarkaraḥ|
avidāhīni cānnāni śōphē bhēṣajamuttamam||48||
pUrvarUpaM bhiShagbuddhvA vraNAnAM shophamAditaH |
raktAvasecanaM kuryAdajAtavraNashAntaye ||44||
shodhayedbahudoShAMstu svalpadoShAn vila~gghayet |
pUrvaM kaShAyasarpirbhirjayedvA mArutottarAn ||45||
nyagrodhodumbarAshvatthaplakShavetasavalkalaiH |
sasarpiShkaiH pralepaH syAcchophanirvApaNaH param ||46||
vijayA madhukaM vIrA bisagranthiH shatAvarI |
nIlotpalaM nAgapuShpaM pradehaH syAt sacandanaH ||47||
saktavo madhukaM sarpiH pradehaH syAt sasharkaraH |
avidAhIni cAnnAni shophe bheShajamuttamam ||48||
The physician observing shopha (swelling) as prodromal sign in the beginning should apply blood-letting to prevent the manifestation of wound. One should evacuate the persons with plenty of impurity and lighten those with little impurity. He should overcome the wound predominant in vata first with decoctions and ghritas. Paste of nyogrodha bark (Ficus bengalensis Linn.), udumbara (Ficus glomerata Roxb.), ashwattha (Ficus religiosa Linn.), plaksha (Ficus lacor Buch.Ham.) and vetasa (Salix caprea Linn.) are mixed with ghee is an excellent cooling for inflammation, other local applications prescribed are (1) vijaya (Terminalia chebula Retz.), madhuka (Glycyrrhiza glabra Linn.), vira , bisagranthi, shatavari (Asparagus racemosus Willd.), nilotpala (Nymphea stellata Willd.), nagapuspa (Mesua ferrea Linn.) and sandal (Santalum album Linn.). (2) Parched grain flour, madhuka, sarkara and ghee. Avidahi (non-burning) food is the best remedy for inflammation.[44-48]
Patana (incision) and upanaha (poultice)
स चेदेवमुपक्रान्तः शोफो न प्रशमं व्रजेत् |
तस्योपनाहैः पक्वस्य पाटनं हितमुच्यते ||४९||
तैलेन सर्पिषा वाऽपि ताभ्यां वा सक्तुपिण्डिका |
सुखोष्णा शोफपाकार्थमुपनाहः प्रशस्यते ||५०||
सतिला सातसीबीजा दध्यम्ला सक्तुपिण्डिका |
सकिण्वकुष्ठलवणा शस्ता स्यादुपनाहने ||५१||
रुग्दाहरागतोदैश्च विदग्धं शोफमादिशेत् |
जलबस्तिसमस्पर्शं सम्पक्वं पीडितोन्नतम् ||५२||
उमाऽथो गुग्गुलुः सौधं पयो दक्षकपोतयोः |
विट् पलाशभवः क्षारो हेमक्षीरी मुकूलकः ||५३||
इत्युक्तो भेषजगणः पक्वशोथप्रभेदनः |
सुकुमारस्य, कृच्छ्रस्य शस्त्रं तु परमुच्यते ||५४||
sa cēdēvamupakrāntaḥ śōphō na praśamaṁ vrajēt|
tasyōpanāhaiḥ pakvasya pāṭanaṁ hitamucyatē||49||
tailēna sarpiṣā vā'pi tābhyāṁ vā saktupiṇḍikā|
sukhōṣṇā śōphapākārthamupanāhaḥ praśasyatē||50||
satilā sātasībījā dadhyamlā saktupiṇḍikā|
sakiṇvakuṣṭhalavaṇā śastā syādupanāhanē||51||
rugdāharāgatōdaiśca vidagdhaṁ śōphamādiśēt|
jalabastisamasparśaṁ sampakvaṁ pīḍitōnnatam||52||
umā'thō gugguluḥ saudhaṁ payō dakṣakapōtayōḥ|
viṭ palāśabhavaḥ kṣārō hēmakṣīrī mukūlakaḥ||53||
ityuktō bhēṣajagaṇaḥ pakvaśōthaprabhēdanaḥ|
sukumārasya, kr̥cchrasya śastraṁ tu paramucyatē||54||
sa cedevamupakrAntaH shopho na prashamaM vrajet |
tasyopanAhaiH pakvasya pATanaM hitamucyate ||49||
tailena sarpiShA vA~api tAbhyAM vA saktupiNDikA |
sukhoShNA shophapAkArthamupanAhaH prashasyate ||50||
satilA sAtasIbIjA dadhyamlA saktupiNDikA |
sakiNvakuShThalavaNA shastA syAdupanAhane ||51||
rugdAharAgatodaishca vidagdhaM shophamAdishet |
jalabastisamasparshaM sampakvaM pIDitonnatam ||52||
umA~atho gugguluH saudhaM payo dakShakapotayoH |
viT palAshabhavaH kShAro hemakShIrI mukUlakaH ||53||
ityukto bheShajagaNaH pakvashothaprabhedanaH |
sukumArasya, kRucchrasya shastraM tu paramucyate ||54||
If swelling of ulcers treated in this way does not subside, poultice should be applied and when ripened should be incised. Warm poultice of the bolus of parched grain flour mixed with oil or ghee or both is useful for ripening of inflammation. The bolus of parched grain flour mixed with tila (Sesamum indicum Linn.), linseeds (Linum usitatissimum Linn.), sour curd, yeast, kustha (Saussurea lappa C. B. Clarke) and salt is recommended as poultice.
Swelling is known as vidagdha (under ripening) by the symptoms such as pain, burning sensation, redness and piercing pain. The same should be known as ripened when it is like water-bag on palpation and rises on pressure. Linseed, guggulu (Commiphora mukul), latex of snuhi (Euphorbia neriifolia Linn.), feces of chicken and pigeon, alkali of palasha (Butea monosperma Linn.), svarnakhsiri (Argemone mexicana Linn.) and mukulaka (Pistacia vera Linn.). This is the group of drugs which helps in the tearing of ripened inflammation in delicate patients otherwise it should be operated upon surgically.[49-54]
Six types of surgical procedures
पाटनं व्यधनं चैव छेदनं लेपनं तथा |
प्रच्छनं सीवनं चैव षङ्विधं शस्त्रकर्म तत् ||५५||
pāṭanaṁ vyadhanaṁ caiva chēdanaṁ lēpanaṁ tathā|
pracchanaṁ sīvanaṁ caiva ṣaḍvidhaṁ śastrakarma tat||55||
pATanaM vyadhanaM caiva chedanaM lepanaM tathA |
pracchanaM sIvanaM caiva Sha~gvidhaM shastrakarma tat ||55||
Surgical treatment is of six types such as – incision, puncturing, excision, scrapping, scarification and suturing.[55]
Indications of various surgical procedures
नाडीव्रणाः पक्वशोथास्तथा क्षतगुदोदरम् |
अन्तःशल्याश्च ये शोफाः [१] पाट्यास्ते तद्विधाश्च ये ||५६||
दकोदराणि सम्पक्वा गुल्मा ये ये च रक्तजाः |
व्यध्याः शोणितरोगाश्च विसर्पपिडकादयः ||५७||
उद्वृत्तान् स्थूलपर्यन्तानुत्सन्नान् कठिणान् व्रणान् |
अर्शःप्रभृत्यधीमांसं छेदनेनोपपादयेत् ||५८||
किलासानि सकुष्ठानि लिखेल्लेख्यानि बुद्धिमान् |
वातासृग्ग्रन्थिपिडकाः सकोठा रक्तमण्डलम् ||५९||
कुष्ठान्यभिहतं चाङ्गं शोथांश्च प्रच्छयेद्भिषक् |
सीव्यं कुक्ष्युदराद्यं तु गम्भीरं यद्विपाटितम् ||६०||
इति षड्विधमुद्दिष्टं शस्त्रकर्म मनीषिभिः |६१|
nāḍīvraṇāḥ pakvaśōthāstathā kṣatagudōdaram|
antaḥśalyāśca yē śōphāḥ [1] pāṭyāstē tadvidhāśca yē||56||
dakōdarāṇi sampakvā gulmā yē yē ca raktajāḥ|
vyadhyāḥ śōṇitarōgāśca visarpapiḍakādayaḥ||57||
udvr̥ttān sthūlaparyantānutsannān kaṭhiṇān vraṇān|
arśaḥprabhr̥tyadhīmāṁsaṁ chēdanēnōpapādayēt||58||
kilāsāni sakuṣṭhāni likhēllēkhyāni buddhimān|
vātāsr̥ggranthipiḍakāḥ sakōṭhā raktamaṇḍalam||59||
kuṣṭhānyabhihataṁ cāṅgaṁ śōthāṁśca pracchayēdbhiṣak|
sīvyaṁ kukṣyudarādyaṁ tu gambhīraṁ yadvipāṭitam||60||
iti ṣaḍvidhamuddiṣṭaṁ śastrakarma manīṣibhiḥ|61|
nADIvraNAH pakvashothAstathA kShatagudodaram |
antaHshalyAshca ye shophAH [1] pATyAste tadvidhAshca ye ||56||
dakodarANi sampakvA gulmA ye ye ca raktajAH |
vyadhyAH shoNitarogAshca visarpapiDakAdayaH ||57||
udvRuttAn sthUlaparyantAnutsannAn kaThiNAn vraNAn |
arshaHprabhRutyadhImAMsaM chedanenopapAdayet ||58||
kilAsAni sakuShThAni likhellekhyAni buddhimAn |
vAtAsRuggranthipiDakAH sakoThA raktamaNDalam ||59||
kuShThAnyabhihataM cA~ggaM shothAMshca pracchayedbhiShak |
sIvyaM kukShyudarAdyaM tu gambhIraM yadvipATitam ||60||
iti ShaDvidhamuddiShTaM shastrakarma manIShibhiH |61|
Sinuses, ripened inflammations (i.e.suppurated ulcer or abscess), intestinal perforation, intestinal obstruction, having foreign body within and other similar conditions are incisable. Ascites, suppurated tumor and raktaja gulma (uterine tumor), blood disorders such as erysipelas, boils etc, are treated by puncturing. Wounds protruded with thick margins, elevated, hard, piles etc and other growths should be excised.The wise physician should scrape leucoderma, skin diseases and other such disorders which need scraping. The physician should perform scarification over vatarakta(nodular swelling), granthi (cysts) pimples, urticarial rashes, red patches, skin diseases, injured parts and swellings. Suturing should be done in pelvic, abdominal surgeries (i.e., laparotomy) etc.Thus the scholars have mentioned six types of surgical treatments.[56-61]
Vrana pidana(pressing of wound)
सूक्ष्माननाः कोषवन्तो ये व्रणास्तान्प्रपीडयेत् ||६१||
कलायाश्च मसूराश्च गोधूमाः सहरेणवः |
कल्कीकृताः प्रशस्यन्ते निःस्नेहा व्रणपीडने ||६२||
sūkṣmānanāḥ kōṣavantō yē vraṇāstānprapīḍayēt||61||
kalāyāśca masūrāśca gōdhūmāḥ saharēṇavaḥ|
kalkīkr̥tāḥ praśasyantē niḥsnēhā vraṇapīḍanē||62||
sUkShmAnanAH koShavanto ye vraNAstAnprapIDayet ||61||
kalAyAshca masUrAshca godhUmAH sahareNavaH |
kalkIkRutAH prashasyante niHsnehA vraNapIDane ||62||
Wounds with narrow opening and multiple loculi should be pressed on. Kalaya (Pisum sativum Linn.), masura (Lens culinaris Medic.), wheat (Triticum sativum Lam.) and peas pounded and applied as paste without mixing any fat are useful for pressing the wound.[61-62]
Various treatment modalities for pacification of ulcer
शाल्मलीत्वग्बलामूलं तथा न्यग्रोधपल्लवाः |
न्यग्रोधादिकमुद्दिष्टं बलादिकमथापि वा ||६३||
आलेपनं निर्वपणं तद्विद्यात्तैश्च [१] सेचनम् |
सर्पिषा शतधौतेन पयसा मधुकाम्बुना ||६४|
निर्वापयेत् सुशीतेन रक्तपित्तोत्तरान् व्रणान् |६५|
śālmalītvagbalāmūlaṁ tathā nyagrōdhapallavāḥ|
nyagrōdhādikamuddiṣṭaṁ balādikamathāpi vā||63||
ālēpanaṁ nirvapaṇaṁ tadvidyāttaiśca [1] sēcanam|
sarpiṣā śatadhautēna payasā madhukāmbunā||64||
nirvāpayēt suśītēna raktapittōttarān vraṇān|65|
shAlmalItvagbalAmUlaM tathA nyagrodhapallavAH |
nyagrodhAdikamuddiShTaM balAdikamathApi vA ||63||
AlepanaM nirvapaNaM tadvidyAttaishca [1] secanam |
sarpiShA shatadhautena payasA madhukAmbunA ||64||
nirvApayet sushItena raktapittottarAn vraNAn |65|
Bark of shalmali (Salmalia malabarica Schott), bala (Sida cordifolia) root, tender leaves of nyagrodha – this group (of drugs) known as nyagrodhadi or baladi acts as cooling agent applied as paste and sprinkling. Wounds predominant in raktapitta should be cooled by applying very cold ghee washed hundred times, milk or decoction of madhuka (Madhuka indica).[63-65]
लम्बानि व्रणमांसानि प्रलिप्य मधुसर्पिषा ||६५||
सन्दधीत समं वैद्यो बन्धनैश्चोपपादयेत् |
तान्समान्सुस्थिताञ्ज्ञात्वा फलिनीलोध्रकट्फलैः ||६६||
समङ्गाधातकीयुक्तैश्चूर्णितैरवचूर्णयेत् |
पञ्चवल्कलचूर्णैर्वा शुक्तिचूर्णसमायुतैः ||६७||
धातकीलोध्रचूर्णैर्वा तथा रोहन्ति ते व्रणाः |६८|
lambāni vraṇamāṁsāni pralipya madhusarpiṣā||65||
sandadhīta samaṁ vaidyō bandhanaiścōpapādayēt|
tānsamānsusthitāñjñātvā phalinīlōdhrakaṭphalaiḥ||66||
samaṅgādhātakīyuktaiścūrṇitairavacūrṇayēt|
pañcavalkalacūrṇairvā śukticūrṇasamāyutaiḥ||67||
dhātakīlōdhracūrṇairvā tathā rōhanti tē vraṇāḥ|68|
lambAni vraNamAMsAni pralipya madhusarpiShA ||65||
sandadhIta samaM vaidyo bandhanaishcopapAdayet |
tAnsamAnsusthitA~jj~jAtvA phalinIlodhrakaTphalaiH ||66||
sama~ggAdhAtakIyuktaishcUrNitairavacUrNayet |
pa~jcavalkalacUrNairvA shukticUrNasamAyutaiH ||67||
dhAtakIlodhracUrNairvA tathA rohanti te vraNAH |68|
Chronic wound should be pasted with honey and ghee there after bandaged leads to evenly union.When they are evenly set, powder of priyangu (Callicarpa macrophylla Vahl.), lodhra (Symplocos racemosa Roxb.), katphala (Myrica esculenta Buch-Ham.), lajjalu (Mimosa pudica Linn.) and dhataki (Woodfordia fruticosa Kurz.) should be applied thereon or the powder of panchavalkala mixed with that of sukti bhasma (pearl ash) or the powder of dhataki and lodhra should be applied.
Application of above measures leads to proper wounds healing.[65-68]
Management of bone fracture and dislocation
अस्थिभग्नं च्युतं सन्धिं सन्दधीत समं पुनः ||६८||
समेन सममङ्गेन कृत्वाऽन्येन विचक्षणः |
स्थिरैः कवलिकाबन्धैः कुशिकाभिश्च संस्थितम् ||६९||
पट्टैः प्रभूतसर्पिष्कैर्बध्नीयादचलं सुखम् |
अविदाहिभिरन्नैश्च पैष्टिकैस्तमुपाचरेत् ||७०||
ग्लानिर्हि न हिता तस्य सन्धिविश्लेषकारिका |
विच्युताभिहताङ्गानां विसर्पादीनुपद्रवान् ||७१||
उपाचरेद्यथाकालं [१] कालज्ञः स्वाच्चिकित्सितात् |७२|
asthibhagnaṁ cyutaṁ sandhiṁ sandadhīta samaṁ punaḥ||68||
samēna samamaṅgēna kr̥tvā'nyēna vicakṣaṇaḥ|
sthiraiḥ kavalikābandhaiḥ kuśikābhiśca saṁsthitam||69||
paṭṭaiḥ prabhūtasarpiṣkairbadhnīyādacalaṁ sukham|
avidāhibhirannaiśca paiṣṭikaistamupācarēt||70||
glānirhi na hitā tasya sandhiviślēṣakārikā|
vicyutābhihatāṅgānāṁ visarpādīnupadravān||71||
upācarēdyathākālaṁ [1] kālajñaḥ svāccikitsitāt|72|
asthibhagnaM cyutaM sandhiM sandadhIta samaM punaH ||68||
samena samama~ggena kRutvA~anyena vicakShaNaH |
sthiraiH kavalikAbandhaiH kushikAbhishca saMsthitam ||69||
paTTaiH prabhUtasarpiShkairbadhnIyAdacalaM sukham |
avidAhibhirannaishca paiShTikaistamupAcaret ||70||
glAnirhi na hitA tasya sandhivishleShakArikA |
vicyutAbhihatA~ggAnAM visarpAdInupadravAn ||71||
upAcaredyathAkAlaM [1] kAlaj~jaH svAccikitsitAt |72|
Fractured bone and dislocated joints should be set correctly comparing with its counterpart. Setting with firm pad-bandages and splints, it should be immobilized without any discomfort by binding with cloth pieces dipped in plenty of ghee. The patient should be kept on non-burning foods (avidahi) made of flour. Such patients should not resort to physical exercise which may cause dislocation of joint. The physician, according to time, should treat the complications such as erysipelas etc in fracture and dislocation of bone. [68-72]
Management of various conditions of vrana
शुष्का महारुजः स्तब्धा ये व्रणा मारुतोत्तराः |
स्वेद्याः सङ्करकल्पेन ते स्युः कृशरपायसैः ||७२||
ग्राम्यबैलाम्बुजानूपैर्वैशवारैश्च संस्कृतैः |
उत्कारिकाभिश्चोष्णाभिः सुखी स्याद्व्रणितस्तथा ||७३||
सदाहा वेदनावन्तो ये व्रणा मारुतोत्तराः |
तेषामुमां तिलांश्चैव भृष्टान् पयसि निर्वृतान् ||७४||
तेनैव पयसा पिष्ट्वा कुर्यादालेपनं भिषक् |
बला गुडूची मधुकं पृश्निपर्णी शतावरी ||७५||
जीवन्ती शर्करा क्षीरं तैलं मत्स्यवसा घृतम् |
संसिद्धा समधूच्छिष्टा शूलघ्नी स्नेहशर्करा ||७६||
द्विपञ्चमूलक्वथितेनाम्भसा पयसाऽथवा [१] |
सर्पिषा वा सतैलेन कोष्णेन परिषेचयेत् ||७७||
यवचूर्णं समधुकं सतिलं सह सर्पिषा |
दद्यादालेपनं कोष्णं दाहशूलोपशान्तये ||७८||
उपनाहश्च कर्तव्यः सतिलो मुद्गपायसः |
रुग्दाहयोः प्रशमनो व्रणेष्वेष विधिर्हितः ||७९||
śuṣkā mahārujaḥ stabdhā yē vraṇā mārutōttarāḥ|
svēdyāḥ saṅkarakalpēna tē syuḥ kr̥śarapāyasaiḥ||72||
grāmyabailāmbujānūpairvaiśavāraiśca saṁskr̥taiḥ|
utkārikābhiścōṣṇābhiḥ sukhī syādvraṇitastathā||73||
sadāhā vēdanāvantō yē vraṇā mārutōttarāḥ|
tēṣāmumāṁ tilāṁścaiva bhr̥ṣṭān payasi nirvr̥tān||74||
tēnaiva payasā piṣṭvā kuryādālēpanaṁ bhiṣak|
balā guḍūcī madhukaṁ pr̥śniparṇī śatāvarī||75||
jīvantī śarkarā kṣīraṁ tailaṁ matsyavasā ghr̥tam|
saṁsiddhā samadhūcchiṣṭā śūlaghnī snēhaśarkarā||76||
dvipañcamūlakvathitēnāmbhasā payasā'thavā [1] |
sarpiṣā vā satailēna kōṣṇēna pariṣēcayēt||77||
yavacūrṇaṁ samadhukaṁ satilaṁ saha sarpiṣā|
dadyādālēpanaṁ kōṣṇaṁ dāhaśūlōpaśāntayē||78||
upanāhaśca kartavyaḥ satilō mudgapāyasaḥ|
rugdāhayōḥ praśamanō vraṇēṣvēṣa vidhirhitaḥ||79||
shuShkA mahArujaH stabdhA ye vraNA mArutottarAH |
svedyAH sa~gkarakalpena te syuH kRusharapAyasaiH ||72||
grAmyabailAmbujAnUpairvaishavAraishca saMskRutaiH |
utkArikAbhishcoShNAbhiH sukhI syAdvraNitastathA ||73||
sadAhA vedanAvanto ye vraNA mArutottarAH |
teShAmumAM tilAMshcaiva bhRuShTAn payasi nirvRutAn ||74||
tenaiva payasA piShTvA kuryAdAlepanaM bhiShak |
balA guDUcI madhukaM pRushniparNI shatAvarI ||75||
jIvantI sharkarA kShIraM tailaM matsyavasA ghRutam |
saMsiddhA samadhUcchiShTA shUlaghnI snehasharkarA ||76||
dvipa~jcamUlakvathitenAmbhasA payasA~athavA [1] |
sarpiShA vA satailena koShNena pariShecayet ||77||
yavacUrNaM samadhukaM satilaM saha sarpiShA |
dadyAdAlepanaM koShNaM dAhashUlopashAntaye ||78||
upanAhashca kartavyaH satilo mudgapAyasaH |
rugdAhayoH prashamano vraNeShveSha vidhirhitaH ||79||
Wounds which are dry, intensely painful, stiffened and predominant in vata should be fomented by bolus fomentation with krishara and payasa (a type of dietary preparation). Similarly, they should be fomented with seasoned vesavara made of the meat of domestic, burrow-dwellers, aquatic or marshy animals or hot utkarika. Thus the patient gets relief. If the wounds predominant in vata have burning sensation and pain, they should be pasted upon with linseed and sesamum seeds roasted, then dipped in milk and again pounded with the same milk. Bala (Sida cordifolia Linn.), guduchi (Tinospora cordifolia), madhuka (Glycyrrhiza glabra Linn.), prishnaparni (Uraria picta Desv), shatavari (Asparagus racemosus Willd), jivanti (Leptadenia reticulate W. & A.), sugar, milk, oil, fish fat, ghee cooked with beeswax is known as sneha sarkara, it relieves pain.The wound should be sprinkled with warm decoction of two panchamula (ie.dashamula), milk and ghee with oil.
Barley powder (Hordeum vulgare Linn.), madhuka (Glycyrrhiza glabra Linn.) and tila mixed with ghee should be applied as warm paste for alleviating burning sensation and pain. Payasa prepared of mudga (Phaseolus radiates Linn.) mixed with tila should be applied as poultice to pacify pain and burning sensation. These management principles are beneficial in wounds.[72-79]
Eshana (Probing)
सूक्ष्मानना बहुस्रावाः कोषवन्तश्च ये व्रणाः |
न च मर्माश्रितास्तेषामेषणं हितमुच्यते ||८०||
द्विविधामेषणीं विद्यान्मृद्वीं च कठिनामपि |
औद्भिदैर्मृदुभिर्नालैर्लोहानां वा शलाकया ||८१||
गम्भीरे मांसले देशे पाट्यं लौहशलाकया |
एष्यं विद्याद्व्रणं नालैर्विपरीतमतो भिषक् ||८२||
sūkṣmānanā bahusrāvāḥ kōṣavantaśca yē vraṇāḥ|
na ca marmāśritāstēṣāmēṣaṇaṁ hitamucyatē||80||
dvividhāmēṣaṇīṁ vidyānmr̥dvīṁ ca kaṭhināmapi|
audbhidairmr̥dubhirnālairlōhānāṁ vā śalākayā||81||
gambhīrē māṁsalē dēśē pāṭyaṁ lauhaśalākayā|
ēṣyaṁ vidyādvraṇaṁ nālairviparītamatō bhiṣak||82||
sUkShmAnanA bahusrAvAH koShavantashca ye vraNAH |
na ca marmAshritAsteShAmeShaNaM hitamucyate ||80||
dvividhAmeShaNIM vidyAnmRudvIM ca kaThinAmapi |
audbhidairmRudubhirnAlairlohAnAM vA shalAkayA ||81||
gambhIre mAMsale deshe pATyaM lauhashalAkayA |
eShyaM vidyAdvraNaM nAlairviparItamato bhiShak ||82||
In case of wounds with narrow opening, profuse discharge and pouch and not situated in vital parts, probing is beneficial. Probe is of two types – soft and hard, the former is made of soft stalks of plants and the latter of iron (metallic) rods. In deep and muscular parts iron rods preferred while in other parts plant stalks should be used for probing. [80-82]
Vrana shodhana (local purification of ulcers)
पूतिगन्धान् विवर्णांश्च बहुस्रावान्महारुजः |
व्रणानशुद्धान् विज्ञाय शोधनैः समुपाचरेत् ||८३||
त्रिफला खदिरो दार्वी न्यग्रोधादिर्बला [१] कुशः |
निम्बकोलकपत्राणि कषायाः शोधना मताः ||८४||
तिलकल्कः सलवणो द्वे हरिद्रे त्रिवृद्धृतम् |
मधुकं निम्बपत्राणि प्रलेपो व्रणशोधनः ||८५||
pūtigandhān vivarṇāṁśca bahusrāvānmahārujaḥ|
vraṇānaśuddhān vijñāya śōdhanaiḥ samupācarēt||83||
triphalā khadirō dārvī nyagrōdhādirbalā [1] kuśaḥ|
nimbakōlakapatrāṇi kaṣāyāḥ śōdhanā matāḥ||84||
tilakalkaḥ salavaṇō dvē haridrē trivr̥ddhr̥tam|
madhukaṁ nimbapatrāṇi pralēpō vraṇaśōdhanaḥ||85||
pUtigandhAn vivarNAMshca bahusrAvAnmahArujaH |
vraNAnashuddhAn vij~jAya shodhanaiH samupAcaret ||83||
triphalA khadiro dArvI nyagrodhAdirbalA [1] kushaH |
nimbakolakapatrANi kaShAyAH shodhanA matAH ||84||
tilakalkaH salavaNo dve haridre trivRuddhRutam |
madhukaM nimbapatrANi pralepo vraNashodhanaH ||85||
Wounds with foul odor, abnormal color, profuse discharge and intense pain should be known as dushta vrana (unclean) and as such wounds should be treated with cleansing agents. Decoctions of triphala, khadira (Acasia catechu Willd), daruharidra (Berberis aristata DC), nyagrodhadi group, bala (Sida cordifolia Linn.), kusa (Desmostachya bipinnata Stapf.), leaves of nimba (Azadirachta indica A. Juss) and badara (Zizyphus jujube Lam.) are regarded as cleansing drugs. Tila paste, salt, haridra (Curcuma longa Linn.), daruharidra (Berberis aristata DC), trivrit (Operculina turpethum Linn.) ghrita, madhuka, nimba leaves – this formulation is said as wound cleanser. [83-85]
Ropana (healing) of ulcer
नातिरक्तो नातिपाण्डुर्नातिश्यावो न चातिरुक् |
न चोत्सन्नो न चोत्सङ्गी शुद्धो रोप्यः परं व्रणः ||८६||
न्यग्रोधोदुम्बराश्वत्थकदम्बप्लक्षवेतसाः |
करवीरार्ककुटजाः कषाया व्रणरोपणाः ||८७||
चन्दनं पद्मकिञ्जल्कं दार्वीत्वङ्नीलमुत्पलम् |
मेदे मूर्वा समङ्गा च यष्ट्याह्वं व्रणरोपणम् ||८८||
प्रपौण्डरीकं जीवन्ती गोजिह्वा धातकी बला |
रोपणं सतिलं दद्यात् प्रलेपं सघृतं व्रणे ||८९||
कम्पिल्लकं विडङ्गानि वत्सकं त्रिफलां बलाम् |
पटोलं पिचुमर्दं च लोध्रं मुस्तं प्रियङ्गुकम् ||९०||
खदिरं धातकीं सर्जमेलामगुरुचन्दने |
पिष्ट्वा साध्यं भवेत्तैलं तत् परं व्रणरोपणम् ||९१||
प्रपौण्डरीकं मधुकं काकोल्यौ द्वे च चन्दने |
सिद्धमेतैः समैस्तैलं परं स्याद्व्रणरोपणम् ||९२||
दूर्वास्वरससिद्धं वा तैलं कम्पिल्लकेन वा |
दार्वीत्वचश्च कल्केन प्रधानं व्रणरोपणम् ||९३||
येनैव विधिना तैलं घृतं तेनैव साधयेत् |
रक्तपित्तोत्तरं दृष्ट्वा रोपणीयं व्रणं भिषक् ||९४|
nātiraktō nātipāṇḍurnātiśyāvō na cātiruk|
na cōtsannō na cōtsaṅgī śuddhō rōpyaḥ paraṁ vraṇaḥ||86||
nyagrōdhōdumbarāśvatthakadambaplakṣavētasāḥ|
karavīrārkakuṭajāḥ kaṣāyā vraṇarōpaṇāḥ||87||
candanaṁ padmakiñjalkaṁ dārvītvaṅnīlamutpalam|
mēdē mūrvā samaṅgā ca yaṣṭyāhvaṁ vraṇarōpaṇam||88||
prapauṇḍarīkaṁ jīvantī gōjihvā dhātakī balā|
rōpaṇaṁ satilaṁ dadyāt pralēpaṁ saghr̥taṁ vraṇē||89||
kampillakaṁ viḍaṅgāni vatsakaṁ triphalāṁ balām|
paṭōlaṁ picumardaṁ ca lōdhraṁ mustaṁ priyaṅgukam||90||
khadiraṁ dhātakīṁ sarjamēlāmagurucandanē|
piṣṭvā sādhyaṁ bhavēttailaṁ tat paraṁ vraṇarōpaṇam||91||
prapauṇḍarīkaṁ madhukaṁ kākōlyau dvē ca candanē|
siddhamētaiḥ samaistailaṁ paraṁ syādvraṇarōpaṇam||92||
dūrvāsvarasasiddhaṁ vā tailaṁ kampillakēna vā|
dārvītvacaśca kalkēna pradhānaṁ vraṇarōpaṇam||93||
yēnaiva vidhinā tailaṁ ghr̥taṁ tēnaiva sādhayēt|
raktapittōttaraṁ dr̥ṣṭvā rōpaṇīyaṁ vraṇaṁ bhiṣak||94||
| nAtirakto nAtipANDurnAtishyAvo na cAtiruk |
na cotsanno na cotsa~ggI shuddho ropyaH paraM vraNaH ||86||
nyagrodhodumbarAshvatthakadambaplakShavetasAH |
karavIrArkakuTajAH kaShAyA vraNaropaNAH ||87||
candanaM padmaki~jjalkaM dArvItva~gnIlamutpalam |
mede mUrvA sama~ggA ca yaShTyAhvaM vraNaropaNam ||88||
prapauNDarIkaM jIvantI gojihvA dhAtakI balA |
ropaNaM satilaM dadyAt pralepaM saghRutaM vraNe ||89||
kampillakaM viDa~ggAni vatsakaM triphalAM balAm |
paTolaM picumardaM ca lodhraM mustaM priya~ggukam ||90||
khadiraM dhAtakIM sarjamelAmagurucandane |
piShTvA sAdhyaM bhavettailaM tat paraM vraNaropaNam ||91||
prapauNDarIkaM madhukaM kAkolyau dve ca candane |
siddhametaiH samaistailaM paraM syAdvraNaropaNam ||92||
dUrvAsvarasasiddhaM vA tailaM kampillakena vA |
dArvItvacashca kalkena pradhAnaM vraNaropaNam ||93||
yenaiva vidhinA tailaM ghRutaM tenaiva sAdhayet |
raktapittottaraM dRuShTvA ropaNIyaM vraNaM bhiShak ||94||
Those ulcers, are not very red, pale, blackish, painful, elevated and protruded should be known as clean and appeals healing process. Decoction of nyagrodha, udumbara, asvattha, kadamba, plaksha, vetasa, karavira (Nerium indicum Mill.), arka (Calotropis procera R. Br.) and kutaja (Holarrhena antidysentrica Linn.) are wound healing. Chandana (Santalum album Linn.), lotus stamens, daruharidra bark, blue water lily, meda (Polygonatum airrhifolium Royle), mahameda (Polygonatum airrhifolium Royle), murva (Marsdenia tenacissima W. & A.), lajjalu (Mimosa pudica Linn.) and madhuyasti- this formulation is wound healer. Prapaundarika, jivanti, gojihva (Onosma bracteatum Wall.), dhataki, bala and sesamum should be applied as paste with ghee for wound healing. Kampillaka (Mallotus philippinensis Muell Arg), vidanga (Embelia ribes Burm), kutaja, triphala, bala, patola (Trichosanthes dioica Roxb.), nimba, musta (Cyperus rotundus Linn.), priyangu, khadira, dhataki, sarja, ela (Elleteria cardamomum Maton.), aguru (Aquilaria agallocha Roxb.) and chandana are pounded together and oil is extracted. This oil is used as ulcer healing agent.
Similarly, oil prepared with equal quantity of prapaundarika, mahuka, kakoli (Roscoca procera Wall.), kshirakakoli (Roscoca procera Wall.), chandana and rakta chandana (Pterocarpus santalinus Linn.) is an excellent ulcer healing agent. Oil cooked with durva juice or kampillaka or paste of daruharidra bark is an important ulcer healer. By the above method ghrita should be prepared and used for healing, ulcers predominant in rakta and pitta.[86-94]
Patta bandhana (bandage)
कदम्बार्जुननिम्बानां पाटल्याः पिप्पलस्य च |
व्रणप्रच्छादने विद्वान् पत्राण्यर्कस्य चादिशेत् ||९५||
वार्क्षोऽथवाऽऽजिनः क्षौमः पट्टो व्रणहितः स्मृतः |
बन्धश्च द्विविधः शस्तो व्रणानां सव्यदक्षिणः ||९६||
kadambārjunanimbānāṁ pāṭalyāḥ pippalasya ca|
vraṇapracchādanē vidvān patrāṇyarkasya cādiśēt||95||
vārkṣō'thavājinaḥ kṣaumaḥ paṭṭō vraṇahitaḥ smr̥taḥ|
bandhaśca dvividhaḥ śastō vraṇānāṁ savyadakṣiṇaḥ||96||
kadambArjunanimbAnAM pATalyAH pippalasya ca |
vraNapracchAdane vidvAn patrANyarkasya cAdishet ||95||
vArkSho~athavA~a~ajinaH kShaumaH paTTo vraNahitaH smRutaH |
bandhashca dvividhaH shasto vraNAnAM savyadakShiNaH ||96||
For covering the wound, leaves of kadamba, arjuna, nimba, patala (Stereospermum suaveolens DC.), pippala (Ficus religiosa Linn.) and arka should be used. Bandage made of plant bark, deer hide or flaxen cloth is used in wounds. Bandaging of wounds are of two types i.e, It can be started either from left or right side. [95-96]
Contraindications
लवणाम्लकटूष्णानि विदाहीनि गुरूणि च |
वर्जयेदन्नपानानि व्रणी मैथुनमेव च ||९७||
नातिशीतगुरुस्निग्धमविदाहि यथाव्रणम् |
अन्नपानं व्रणहितं हितं चास्वपनं दिवा ||९८||
lavaṇāmlakaṭūṣṇāni vidāhīni gurūṇi ca|
varjayēdannapānāni vraṇī maithunamēva ca||97||
nātiśītagurusnigdhamavidāhi yathāvraṇam|
annapānaṁ vraṇahitaṁ hitaṁ cāsvapanaṁ divā||98||
lavaNAmlakaTUShNAni vidAhIni gurUNi ca |
varjayedannapAnAni vraNI maithunameva ca ||97||
nAtishItagurusnigdhamavidAhi yathAvraNam |
annapAnaM vraNahitaM hitaM cAsvapanaM divA ||98||
Patients of ulcer should abstain from salt, sour, pungent, hot, burning and heavy food and drinks and also sexual intercourse. Food and drinks that are not too cold, heavy and fatty, non-burning, according to the nature of ulcer are beneficial, while day-sleep is not suitable in these patient.[97-98]
Suitable food and medicines
स्तन्यानि जीवनीयानि बृंहणीयानि यानि च |
उत्सादनार्थं निम्नानां व्रणानां तानि कल्पयेत् ||९९||
भूर्जग्रन्थ्यश्मकासीसमधोभागानि गुग्गुलुः |
व्रणावसादनं तद्वत् कलविङ्ककपोतविट् ||१००||
stanyāni jīvanīyāni br̥ṁhaṇīyāni yāni ca|
utsādanārthaṁ nimnānāṁ vraṇānāṁ tāni kalpayēt||99||
bhūrjagranthyaśmakāsīsamadhōbhāgāni gugguluḥ|
vraṇāvasādanaṁ tadvat kalaviṅkakapōtaviṭ||100||
stanyAni jIvanIyAni bRuMhaNIyAni yAni ca |
utsAdanArthaM nimnAnAM vraNAnAM tAni kalpayet ||99||
bhUrjagranthyashmakAsIsamadhobhAgAni gugguluH |
vraNAvasAdanaM tadvat kalavi~gkakapotaviT ||100||
For raising the depressed wounds galactogogues (stanyajanana), vitalizers (jeevaniya) and bulk promotives (brinhaniya) drugs should be applied. Similarly, bhurjagranthi (nodes in the tree of Butea utilis), asmakasisa (copper sulphate), purgatives, guggulu and excrement of sparrow and pigeon should be used for depressing the wounds. [99-100]
Indications and contraindications of agni karma (cauterization)
रुधिरेऽतिप्रवृत्ते तु च्छिन्ने च्छेद्येऽधिमांसके |
कफग्रन्थिषु गण्डेषु वातस्तम्भानिलार्तिषु ||१०१||
गूढपूयलसीकेषु गम्भीरेषु स्थिरेषु च |
कलाप्तेषु [१] चाङ्गदेशेषु कर्माग्नेः सम्प्रशस्यते ||१०२||
मधूच्छिष्टेन तैलेन मज्जक्षौद्रवसाघृतैः |
तप्तैर्वा विविधैर्लोहैर्दहेद्दाहविशेषवित् ||१०३||
रूक्षाणां सुकुमाराणां गम्भीरान्मारुतोत्तरान् |
दहेत् स्नेहमधूच्छिष्टैर्लोहैः क्षौद्रैस्ततोऽन्यथा ||१०४||
बालदुर्बलवृद्धानां गर्भिण्या रक्तपित्तिनाम् |
तृष्णाज्वरपरीतानामबलानां विषादिनाम् ||१०५||
नाग्निकर्मोपदेष्टव्यं स्नायुमर्मव्रणेषु च |
सविषेषु च शल्येषु नेत्रकुष्ठव्रणेषु च ||१०६||
rudhirē'tipravr̥ttē tu cchinnē cchēdyē'dhimāṁsakē|
kaphagranthiṣu gaṇḍēṣu vātastambhānilārtiṣu||101||
gūḍhapūyalasīkēṣu gambhīrēṣu sthirēṣu ca|
kl̥ptēṣu [1] cāṅgadēśēṣu karmāgnēḥ sampraśasyatē||102||
madhūcchiṣṭēna tailēna majjakṣaudravasāghr̥taiḥ|
taptairvā vividhairlōhairdahēddāhaviśēṣavit||103||
rūkṣāṇāṁ sukumārāṇāṁ gambhīrānmārutōttarān|
dahēt snēhamadhūcchiṣṭairlōhaiḥ kṣaudraistatō'nyathā||104||
bāladurbalavr̥ddhānāṁ garbhiṇyā raktapittinām|
tr̥ṣṇājvaraparītānāmabalānāṁ viṣādinām||105||
nāgnikarmōpadēṣṭavyaṁ snāyumarmavraṇēṣu ca|
saviṣēṣu ca śalyēṣu nētrakuṣṭhavraṇēṣu ca||106||
rudhire~atipravRutte tu cchinne cchedye~adhimAMsake |
kaphagranthiShu gaNDeShu vAtastambhAnilArtiShu ||101||
gUDhapUyalasIkeShu gambhIreShu sthireShu ca |
kLLipteShu [1] cA~ggadesheShu karmAgneH samprashasyate ||102||
madhUcchiShTena tailena majjakShaudravasAghRutaiH |
taptairvA vividhairlohairdaheddAhavisheShavit ||103||
rUkShANAM sukumArANAM gambhIrAnmArutottarAn |
dahet snehamadhUcchiShTairlohaiH kShaudraistato~anyathA ||104||
bAladurbalavRuddhAnAM garbhiNyA raktapittinAm |
tRuShNAjvaraparItAnAmabalAnAM viShAdinAm ||105||
nAgnikarmopadeShTavyaM snAyumarmavraNeShu ca |
saviSheShu ca shalyeShu netrakuShThavraNeShu ca ||106||
Excessive hemorrhage after excision, excisable growths, kaphaja nodules, glands, stiffness and disorders due to vata, wounds with hidden pus and lymph, deep and firm; and after amputation of body part, cauterization is prescribed. The expert in cauterization should cauterize the spot with beeswax, oil, marrow, honey, muscle-fat, ghrita or various heated metallic sticks. Wounds deep and predominant in vata and in patients rough and delicate should be cauterized with fat or beeswax otherwise with iron stick or honey. Cauterization should not be applied in children, debilitated, old persons, pregnant women, those suffering from internal hemorrhage, thirst, fever, weak and poisoned persons and in wounds situated at ligaments and vital parts, poisoned, foreign body, ophthalmic and leprotic wounds.[101-106]
Kshara karma (application of alkali) and dhupana(fumigation)
रोगदोषबलापेक्षी मात्राकालाग्निकोविदः |
शस्त्रकर्माग्निकृत्येषु क्षारमप्यवचारयेत् ||१०७||
कठिनत्वं व्रणा यान्ति गन्धैः सारैश्च धूपिताः |
सर्पिर्मज्जवसाधूपैः शैथिल्यं यान्ति हि व्रणाः ||१०८||
रुजः स्रावाश्च गन्धाश्च कृमयश्च व्रणाश्रिताः |
शैथिल्यं मार्दवं चापि धूपनेनोपशाम्यति ||१०९||
लोध्रन्यग्रोधशुङ्गानि खदिरस्त्रिफला घृतम् |
प्रलेपो व्रणशैथिल्यसौकुमार्यप्रसाधनः ||११०||
सरुजः कठिनाः स्तब्धा निरास्रावाश्च ये व्रणाः |
यवचूर्णैः ससर्पिष्कैर्बहुशस्तान् प्रलेपयेत् ||१११||
मुद्गषष्टिकशालीनां पायसैर्वा यथाक्रमम् |
सघृतैर्जीवनीयैर्वा तर्पयेत्तानभीक्ष्णशः ||११२||
rōgadōṣabalāpēkṣī mātrākālāgnikōvidaḥ|
śastrakarmāgnikr̥tyēṣu kṣāramapyavacārayēt||107||
kaṭhinatvaṁ vraṇā yānti gandhaiḥ sāraiśca dhūpitāḥ|
sarpirmajjavasādhūpaiḥ śaithilyaṁ yānti hi vraṇāḥ||108||
rujaḥ srāvāśca gandhāśca kr̥mayaśca vraṇāśritāḥ|
śaithilyaṁ mārdavaṁ cāpi dhūpanēnōpaśāmyati||109||
lōdhranyagrōdhaśuṅgāni khadirastriphalā ghr̥tam|
pralēpō vraṇaśaithilyasaukumāryaprasādhanaḥ||110||
sarujaḥ kaṭhināḥ stabdhā nirāsrāvāśca yē vraṇāḥ|
yavacūrṇaiḥ sasarpiṣkairbahuśastān pralēpayēt||111||
mudgaṣaṣṭikaśālīnāṁ pāyasairvā yathākramam|
saghr̥tairjīvanīyairvā tarpayēttānabhīkṣṇaśaḥ||112||
rogadoShabalApekShI mAtrAkAlAgnikovidaH |
shastrakarmAgnikRutyeShu kShAramapyavacArayet ||107||
kaThinatvaM vraNA yAnti gandhaiH sAraishca dhUpitAH |
sarpirmajjavasAdhUpaiH shaithilyaM yAnti hi vraNAH ||108||
rujaH srAvAshca gandhAshca kRumayashca vraNAshritAH |
shaithilyaM mArdavaM cApi dhUpanenopashAmyati ||109||
lodhranyagrodhashu~ggAni khadirastriphalA ghRutam |
pralepo vraNashaithilyasaukumAryaprasAdhanaH ||110||
sarujaH kaThinAH stabdhA nirAsrAvAshca ye vraNAH |
yavacUrNaiH sasarpiShkairbahushastAn pralepayet ||111||
mudgaShaShTikashAlInAM pAyasairvA yathAkramam |
saghRutairjIvanIyairvA tarpayettAnabhIkShNashaH ||112||
The physician conversant with dose, time and agni (heat) may apply alkali in cases amenable to surgical treatment and cauterization according to severity of disease and morbidity. Wounds attain hardness by being fumigated with aromatic substances and heartwood. The wounds get softened if fumigated with ghrita, marrow or muscle-fat. Through fumigation pain, discharges, odors, maggots, hardness and softness of wounds are removed. Lodhra, leaf-buds of nyagrodha, khadira, triphala and ghrita - this combination used as paste provides looseness and softness in wounds. The wounds which are painful, hard, stiff and without discharge should be pasted frequently with barley powder mixed with ghrita. Wounds may be saturated by applying frequently the paste of payasa (cereals cooked with milk) made of mudga, shashtika and shali rice or jivaniya drugs mixed with ghrita.[110-112]
External applications
ककुभोदुम्बराश्वत्थलोध्रजाम्बवकट्फलैः |
त्वचमाश्वेव गृह्णन्ति त्वक्चूर्णैश्चूर्णिता व्रणाः ||११३||
मनःशिलैला [१] मञ्जिष्ठा लाक्षा च रजनीद्वयम् |
प्रलेपः सघृतक्षौद्रस्त्वग्विशुद्धिकरः परः ||११४||
अयोरजः सकासीसं त्रिफलाकुसुमानि च |
करोति लेपः कृष्णत्वं [२] सद्य एव नवत्वचि ||११५||
कालीयकनताम्रास्थिहेमकान्तारसोत्तमैः [३] |
लेपः सगोमयरसः सवर्णीकरणः परः ||११६||
ध्यामकाश्वत्थनिचुलमूलं लाक्षा सगैरिका |
सहेमश्चामृतासङ्गः कासीसं चेति वर्णकृत् ||११७||
चतुष्पदानां त्वग्लोमखुरशृङ्गास्थिभस्मना |
तैलाक्ता चूर्णिता भूमिर्भवेल्लोमवती पुनः ||११८||
षोडशोपद्रवा ये च व्रणानां परिकीर्तिताः |
तेषां चिकित्सा निर्दिष्टा यथास्वं स्वे चिकित्सिते ||११९||
kakubhōdumbarāśvatthalōdhrajāmbavakaṭphalaiḥ|
tvacamāśvēva gr̥hṇanti tvakcūrṇaiścūrṇitā vraṇāḥ||113||
manaḥśilailā [1] mañjiṣṭhā lākṣā ca rajanīdvayam|
pralēpaḥ saghr̥takṣaudrastvagviśuddhikaraḥ paraḥ||114||
ayōrajaḥ sakāsīsaṁ triphalākusumāni ca|
karōti lēpaḥ kr̥ṣṇatvaṁ [2] sadya ēva navatvaci||115||
kālīyakanatāmrāsthihēmakāntārasōttamaiḥ [3] |
lēpaḥ sagōmayarasaḥ savarṇīkaraṇaḥ paraḥ||116||
dhyāmakāśvatthaniculamūlaṁ lākṣā sagairikā|
sahēmaścāmr̥tāsaṅgaḥ kāsīsaṁ cēti varṇakr̥t||117||
catuṣpadānāṁ tvaglōmakhuraśr̥ṅgāsthibhasmanā|
tailāktā cūrṇitā bhūmirbhavēllōmavatī punaḥ||118||
ṣōḍaśōpadravā yē ca vraṇānāṁ parikīrtitāḥ|
tēṣāṁ cikitsā nirdiṣṭā yathāsvaṁ svē cikitsitē||119||
kakubhodumbarAshvatthalodhrajAmbavakaTphalaiH |
tvacamAshveva gRuhNanti tvakcUrNaishcUrNitA vraNAH ||113||
manaHshilailA [1] ma~jjiShThA lAkShA ca rajanIdvayam |
pralepaH saghRutakShaudrastvagvishuddhikaraH paraH ||114||
ayorajaH sakAsIsaM triphalAkusumAni ca |
karoti lepaH kRuShNatvaM [2] sadya eva navatvaci ||115||
kAlIyakanatAmrAsthihemakAntArasottamaiH [3] |
lepaH sagomayarasaH savarNIkaraNaH paraH ||116||
dhyAmakAshvatthaniculamUlaM lAkShA sagairikA |
sahemashcAmRutAsa~ggaH kAsIsaM ceti varNakRut ||117||
catuShpadAnAM tvaglomakhurashRu~ggAsthibhasmanA |
tailAktA cUrNitA bhUmirbhavellomavatI punaH ||118||
ShoDashopadravA ye ca vraNAnAM parikIrtitAH |
teShAM cikitsA nirdiShTA yathAsvaM sve cikitsite ||119||
By dusting the wounds with the powders of barks of kakubha (Termalia arjuna), udumbara, asvattha, lodhra (Symplocos racemosa Roxb), jambu (Eugenia jambolana Lam) and katphala (Myrica esculenta Buch-Ham) they heals the skin quickly.
Manashila (Realgar), manjishtha, lac, haridra and daruharidra used as paste with ghee and honey is an excellent cleanser of skin.
The paste prepared by bhasmas of iron, kasisa and triphala (haritaki,vibhitaki and amalaki) flowers provide blackness in the newly formed skin quickly.
Kaliyaka (Jateorhiza palmata Miers), nata /tagara (Valeriana wallichii DC), mango seeds, nagakeshara, iron and triphala powder mixed with cow-dung juice make an excellent paste for reviving normal color in skin.
Roots of dhyamaka, ashvattha and nichula (Barringtonia acutangula Linn), lac, gairic(red-ochre), nagakeshara and kasisa – These restore the natural colour of the skin.
The hairless spots are smeared with oil and dusting with the ash of skin, hair, hoof, horns and bone of quadrupeds, reproduces hairs.The treatment of sixteen complications of wounds has been mentioned in their respective contexts.[113-119]
Summary
तत्र श्लोकौ-
द्वौ व्रणौ व्रणभेदाश्च परीक्षा दुष्टिरेव च |
स्थानानि गन्धाः स्रावाश्च सोपसर्गाः क्रियाश्च याः ||१२०||
व्रणाधिकारे सप्रश्नमेतन्नवकमुक्तवान् |
मुनिर्व्याससमासाभ्यामग्निवेशाय धीमते ||१२१||
tatra ślōkau-
dvau vraṇau vraṇabhēdāśca parīkṣā duṣṭirēva ca|
sthānāni gandhāḥ srāvāśca sōpasargāḥ kriyāśca yāḥ||120||
vraṇādhikārē sapraśnamētannavakamuktavān|
munirvyāsasamāsābhyāmagnivēśāya dhīmatē||121||
Now the summing up verses –
Two types of wounds, kinds of wounds, examination of wounds, defects, locations, odors, discharges, complications and treatment modalities are described. These topics after queries have been described in brief as well details by the sage to the wise Agnivesha in the chapter on treatment of wound (Dwivraniya Chikitsa). [120-121]
इत्यग्निवेशकृते तन्त्रे चरकप्रतिसंस्कृते दृढबलसम्पूरिते चिकित्सास्थाने द्विव्रणीयचिकित्सितं नाम पञ्चविंशोऽध्यायः ||२५||
ityagnivēśakr̥tē tantrē carakapratisaṁskr̥tē dr̥ḍhabalasampūritē cikitsāsthānē dvivraṇīyacikitsitaṁ nāmapañcaviṁśō'dhyāyaḥ||25||
ityagniveshakRute tantre carakapratisaMskRute dRuDhabalasampUrite cikitsAsthAne dvivraNIyacikitsitaM nAma pa~jcaviMsho~adhyAyaH ||25||
Tattva Vimarsha (Fundamental Principles)
- Vrana (ulcers) are broadly classified into two types viz. nija (endogenous) and agantu (exogenous).
- The treatment of both types of ulcers is based upon the dosha dominance.
- Endogenous ulcers are caused due to vitiation of dosha located in external pathways.
- The clinical features of vata dominance in ulcer are stiffness, hardness on touch, scanty exudation, excruciating and pricking pain with throbbing and blackish discoloration. It should be treated with sampurana (filling of ulcer cavity), intake of unctuous substances (oleation therapy), unctuous fomentation and poultices, ointments and sprinklings.
- The clinical features of pitta dominant ulcer are excessive thirst, unconsciousness, fever, sweating, burning sensation, impurities at the site of ulcer, tearing and foul smell with discharge pus from ulcer. The treatment includes anointing and sprinkling with cold drugs, intake of sweet and bitter drugs, intake of ghee and purgation.
- The clinical features of kapha dominance in ulcer are sliminess, heaviness, unctuousness, numbness, with mild pain, paleness in color, little slough and prolonged healing. It is treated with anointing and sprinkling with astringent, pungent, dry and hot drugs as well as fasting and digestive measures.
- The two types of ulcers are further divided into twenty types on the basis of distinctive features. Their examination can be done by three ways, signs of excess vitiation at site of ulcer are of twelve types, eight locations, fourteen types of discharges, sixteen complications, twenty four defects and thirty six therapeutic measures.
- Skin, blood vessels, flesh, fat, bone, ligament, vital parts and viscera are involved in the pathogenesis of ulcer.
- The treatment of ulcer is done in two ways viz.1. systemic treatment (internal administration of medicine) and 2. Local treatment of ulcer. The treatment is done with drugs that promote healing, purify body and local site of ulcer.
- The first principle of management of ulcer is body purification through therapeutic emesis, purgation, shastra karma (surgical intervention) or basti (medicated enema) after assessment of condition because the ulcers get healed quickly in those with cleansed body.
- The thirty six measures for treatments of ulcers are those for pacification of swelling, six types of surgical operations, pressing, refrigerating, uniting, fomentation, pacification, probing, cleansing, healing, cleaning paste, healing paste, cleaning oil, healing oil, two types of covering with leaf, two types of bandaging, diet, elevation, two types of cauterization, depression, hardening fumigation, softening fumigation, hardening paste, softening paste, powdering, colorization, healing, repillatory.
- At first, bloodletting therapy is done first to reduce swelling in ulcer. Upanaha (hot poultice) and patana (incision) are done according to stage of ulcer.
- Six types of surgical treatments are incision, puncturing, excision, scrapping, scarification and suturing.
- The contraindications in ulcer patients include salt, sour, pungent, hot, burning and heavy food and drinks, sexual intercourse. Food and drinks that are not too cold, heavy and fatty, non-burning, according to the nature of ulcer are beneficial. Day-sleep is not suitable in these patients.
- Fractured bone and dislocated joints should be set correctly comparing with its counterpart. Setting with firm pad-bandages and splints, it should be immobilized without any discomfort by binding with cloth pieces dipped in plenty of ghee.
Vidhi Vimarsha (Applied Inferences )
Classification of ulcers and causes
As said earlier, ulcers are of two types i.e. nija and agantuja, another classification is clean and infected wound. Nija vrana (endogenous ulcer) are caused by vitiation of dosha in the body or due to disease process. The term sharira desotha (ie.endogenous in origin) is used for morbid factors occurring in the body that cause nija vrana (i.e. endogenous ulcer). While agantuja vrana (exogenous ulcer) are caused by external factors (trauma or surgical intervention) like wound caused by stab injury, poisons, fire and sharp weapons or excessive tying of that organ (bandha) etc. In exogenous ulcers, vitiation of dosha occurs later. Nija vrana i.e. vataja, pittaja, kaphaja, raktaja and sannipataja, are caused due to faulty habit, mode of living and seasonal variation. These vitiated dosha, after a series of pathological processes (shada-kriyakala) get lodged at particular site resulting in the formation of vrana.
Samprapti (pathogenesis of vrana): based on shadakriya kala
Clinical pictures of vrana
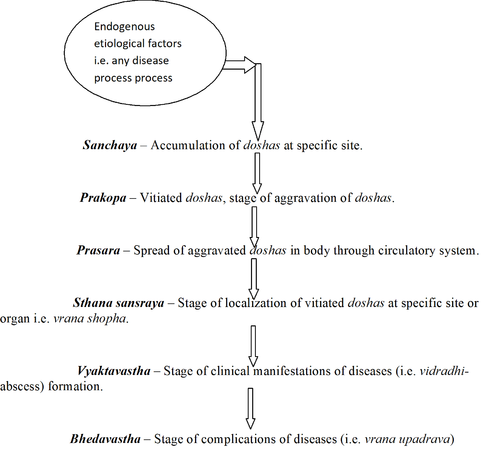
The following ulcer is the case of diabetic ulcer. Clinical features include throbbing pain, swelling, redness, necrosis of involved tissue and non healing ulcer since 6 months.
Image 1: Vata dominant ulcer
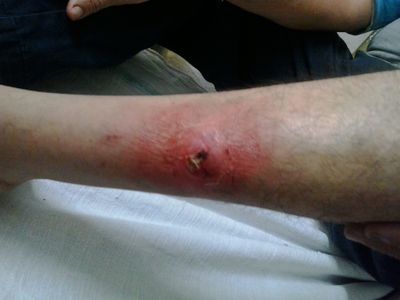
The following ulcer is the case of non healing ulcer due to boils. Clinical features include burning pain, redness, pus discharge, slough, with redness of involved tissue and non healing ulcer since 1month.
Image 2: Pitta dominant ulcer
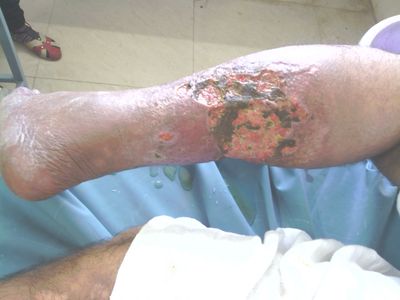
The following ulcer is the case of non healing ulcer due to DCT (Deep vein thrombosis). Clinical features include pain, irregular superficial ulcer, redness, mild pus discharge, slough, with redness of involved tissue and non healing ulcer since 8 months.
Image 3: Kapha dominant ulcer
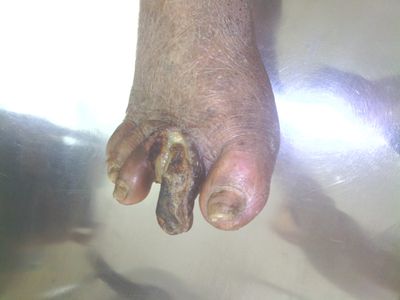
The following ulcer is the case of infected diabetic non healing ulcer (Diabetic foot). Clinical features include severe burning pain, black coloration of first toe with pus discharge, slough, bad smell and deformity in great toe. This is non healing ulcer since 2 months.
Image 4: Dushta vrana
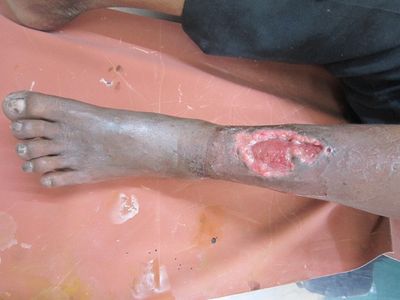
The following ulcer is the case of healing traumatic ulcer at anterior part of tibia/lower leg.. Clinical features include mild pain, no discharge, and margins and thick and inflamed due to their chronic nature and the granulation tissue are seen at base of ulcer. So this is a healing ulcer.
Image 5: Shuddha vrana
Investigations and their clinical interpretation in brief
The clinical features of ulcers are ulceration /disccontineous of skin, discharge (pus/blood/ serum), bad odor, differenct size, painful/painless ulcers. The above symptoms are described by Acharya Sushruta (gandha, varna, sava, vedana, akruti). On the basis of which kind of ulcer (varicose ulcer, diabetic ulcer, arterial ulcer, bedsores, leprotic ulcer, rodent ulcer, etc) the symptoms may vary. In all types of ulcers on the basis of history and clinical examinations the following investigations play important role in diagnosis and prognosis of the Ulcer. TLC (Total leucocyte count), Hb% , Serum crestnine, BSL (Blood sugar level) swab culture, X-ray of affected part if chronic ulcer. If TLC are increase than normal range suggest the acute infection. if Hb% is low then the ulcer will heal delay due hyposia to the tissue. If serum creatinine is increased that might be due to kidney problem which hampered healing of ulcer. In diabetic patients BSL assessment is important for healing as glucose liden tissue are reluctant to heal. Swab culture of wound discharge is necessary to know the organism. Lastly s-xay is essential to know extension of wound upto bone/osteomylituis.
Complications of ulcer
If ulcer is not treated properly it may lead to local and systemic infection leading to septicemia. The tissue necrosis leads to gangrene which further need to amputation.
Causes of non-healing
Two factors mainly affect the process of wound healing viz. local factors and systemic factors.
Local factors are infection, necrosis, foreign body, vascular insufficiency, lymphatic obstruction, continuous movement of part. Systemic causes include old age, protein deficiency, vit-c and zinc deficiency, diabetes mellitus.
Treatment of vrana (ulcers)
Purification measures
Purificatory measures eliminate toxic material from body and improve healing process of ulcer. In case of endogenous ulcer removal of morbid matters (i.e. doshaja) emesis through upward route, purgation through downward route are advised. Other purificatory measures like oleation therapy, sudation therapy should be done prior to emesis, purgation etc. For local purification of ulcer, venesection and vrana basti should be done.Raktamokshana is an important modality[4] indicated predominantly in local vitiation of rakta as in dushta vrana. So along with emesis and purgation blood letting is also important treatment modalities with the help of jalauka (leech application), veinpuncture etc.
Selection of therapeutic measures is done as per condition of vrana and patient.
Thirty six treatment measures
Thirty six types of therapeutic measures are described for the treatment of ulcer. Sixty types of treatment measures are described under the head of shashtiupakrama regarding ulcer treatment.[5] It is not necessary that all the thirty six or sixty therapeutic measures have to be applied in treating an ulcer. I A patient at a time 1 or 4 type of procedures are essential in single case of vrana according to condition of the wound.[5]
In early stage of ulcer only inflammation appears. At this stage bloodletting should be done to break the further manifestation of ulcer. Purificatory measures should be performed in excessively aggravated doshas while lightning measures should be adopted if dosha are less aggravated. In the beginning of edema, therapeutic measures aimed to alleviate aggravated vata followed by other doshaviz. pitta and kapha are advised. Application of various pastes made of vijaya, madhuka, vira, bisagranthi etc. also reduce edema. Edema reducing dietary regimen like light food and food that does not cause burning sensation (avidahi) should be followed.
Indications and process of six fold surgical procedures
Six types of surgical procedures are described for treatment of ulcer such as patana (incision), vyadhana (puncturing), chhedana (excision), lekhana (scrapping), pracchana (scarification) and seevana (suturing). Patana procedure described by Charak is same as for bhedana by Sushruta. Any similar or new procedure can be applied in wound management as per the surgeon’s freedom. [6]
Pidana (Compression)
Widening of external opening (mouth) of ulcer or abscess along with breaking of multiple loculi to make uniform cavity, to avoid the collection of pus in multiple pockets and facilitate free drainage of pus. Pidana (compression) is also helpful to squeeze out the collected pus. For compression various pastes are applied over the ulcer of abscess except on mouth openings.
Management of fracture and dislocation
The basic guidelines for management of fracture and dislocation are to stabilize the fractured bone or dislocated joint by application of splints. Proper alignment of bone is mandatory for healing of fractured bones.[7] Suitable dietary regimen should be followed with avoidance of vidahi (food which causes burning sensation) food.[8] Strenuous exercise is not allowed during healing period due to risk of re-fracture and dislocation. Complications due to fracture of bone or dislocation of joint are managed as per condition. For e.g. If ulcer is due to fracture of bone then treatment of ulcer along with fracture management should be adopted.
Eshanakarma (probing)
It is used in ulcer of narrow opening with expanded base (eg.undermined ulcers). Various types of probes are used in ulcer to know the direction of tract or cavity, depth and discharge from ulcer or sinuses. Generally probing is not done if ulcer is located at vital organs (marma sthana) but in specific conditions as in fistula in ano it can be performed. As per site of ulcer various probes either hard or soft can be used. If deep seated and located at fleshy area hard probe (metallic) is used, in superficially seated ulcers soft probe is used. Probing is essential to know the depth of wound particularly in nadivrana (sinus at any part of the body) or fistula (fistula-in ano is one kind).[9]
Vrana shodhana (cleaning of ulcer)
Cleaning of ulcer is done with shodhana drugs (cleansing agents) leads to vrana ropana (wound healing) process. If ulcer is contaminated i.e.presence of infection causing vectors, profuse secretion, presence of slough etc, in these conditions purificatory measures like debridement of ulcer (i.e. removal of slough), irrigation with shodhana kashaya or paste (purificatory measures) should be applied. Once ulcer becomes clean, healthy granulation tissue formation starts. To enhance and protect the granulation tissue vrana ropana drugs (healing drugs) either externally or internally or in combination are used.
Bandaging material, methods and its applicability in vrana (wound)
Bandaging of wound is very important as it stabilizes wounded part, prevents external injury, prevents contamination from external sources and enhances healing process. Bandaging should not be too tight, nor too loose. Act of bandaging may be from right or left side while others have mentioned fourteen types[10]and fifteen types. [11]
Diet: Wholesome and unwholesome aahar-vihar and ulcer healing promoters
Lavana is vishyandi i. e. producing more secretions from tissues; it aggravates kapha and pitta and mitigates vata[12]
Due to kapha and pitta vitiating properties it causes sliminess (kledana) and burning pain. Excessive lavana, amla and katu rasa will provoke vata dosha and may produce various types of pain. Vidahi food also leads to burning sensation due to srotorodha while sexual intercourse leads to dhatukshaya and aggravates [[vata].] [ Cha. Sa. Chikitsa Sthana 28/59 ], [ Cha. Sa. Vimana Sthana 5/24].
Day time sleep causes srotorodha and gives rise to vitiation of kapha that leads to swelling. Elevation of depressed ulcer is very important aspect of healing process. In Ayurvedic classics stanya janana (galactogogue),[Cha. Sa. Sutra Sthana 4/17 ] jeevaniya (life promoters e.g. vitamins) [ Cha. Sa. Sutra Sthana 4/1 ] and brimhaniya gana (nourishing drugs) [ Cha. Sa. Sutra Sthana 4/2] are described. All these drugs have nutritional value (dhatu poshana) that helps in ulcer healing.
Indications and contraindications of agnikarma (cauterization) in various disorders
Agni karma (cauterization by application of heat) is used as precaution for excessive bleeding ulcers, excision of hanging flesh, kaphaja granthi (enlarged gland due to kapha), goitre and in stiffness (associated with vata) etc. Agnikarma has ushna guna (hot property) which is opposite to vata and kapha. Due to heat, vasodilation leads to alleviation of srotorodha resulting in proper vascularity to organ or part. Dahakarma (cauterization) causes constriction of blood vessels so prevents bleeding from ulcer.[13]Cauterization is performed with the help of many substances like unctuous or ununctous substances etc by many ways e.g. Small spot (bindu), shape of ring (valaya) etc depending on nature of disease, strength of patient and time of application.
Importance of dhupana karma (fumigation therapy) in wound sterilization healing process
Fumigation of ulcer is done with dhupana dravyas (fumigating materials).[14],
[15]. Purpose of fumigation is to make suitable conditions for better ulcer healing such as local sterilization, vasodilation, decreased discharge and removal of foul smell.
Fumigation also relieves pain, discharge and kills microorganisms due to vata, [[kapha] ]alleviating property along with antiseptic property.Various types of preparations are used to harden or soften the wounds as per condition of wound.
- Research studies on management of ulcers: The physician observing inflammation as prodromal sign in the beginning should apply blood-letting to prevent the manifestation of wound. Sushruta also indicated blood letting in initial stage of abscess or inflammatory conditions and in ischemic condition of the wound.[16],[17]
- The nagrodhyadi group is indicated in wound as cooling for wounds which is found healing potential in one research.[18]
- The panchavakkal (Vata (Ficus bengalensis Linn), Udumbara (Ficus glomerata Roxb.), Ashvattha (Ficus religiosa Linn.), Parisha/Pāriśa (Thespesia populenoides L.) and Plaksha (Ficus lacor Buch Ham.),) is indicated for the healing of chronic wound. In resent studies panchavalkal has anti-inflammatory, cleaning and healing potential in some research studies carried out and published in reputed journals of Ayurveda.[19],[20],[21], [22], [23],[24]
- Bala (Sida cordifolia Linn.), guduchi (Tinospora cordifolia), madhuka (Glycyrrhiza glabra Linn.), prshnaparni (Uraria picta Desv), satavari (Asparagus racemosus Willd), jivanti (Leptadenia reticulate W. & A.), sugar, milk, oil, fish fat, ghee cooked with beeswax is known as sneha sarkara, it relieves pain. Some studies have highlighted the wound healing potential of honey mixed with above drugs. [25],[26]Various preparations containing following herbal drugs have wound cleaning effect in single and combination of drugs. The recent studies showed their efficacy as evidence based. Leaves of nimb (Azadirachta indica A. Juss)[27],[28],[29],[30] and haridra (Curcuma longa Linn.) are mentioned as the shodhan and ropan(healing) of wound. [31],[32],[33] The daruharidra (Berberis aristata DC) also showed antimicrobial effect. [34]Wounds with foul odor, abnormal colour, profuse discharge and intense pain should be known as dusta vrana (unclean) and as such wounds should be treated with cleansing agents. Decoctions of triphala, khadira (Acasia catechu Willd), daruharidra (Berberis aristata DC), nyagrodhadi group, bala (Sida cordifolia Linn.), kusa (Desmostachya bipinnata Stapf.), leaves of nimb (Azadirachta indica A. Juss) and badara (Zizyphus jujube Lam.) are regarded as cleansing drugs. Tila paste, salt, haridra (Curcuma longa Linn.), daruharidra (Berberis aristata DC), trivrit (Operculina turpethum Linn.) ghrita, madhuka, nimba leaves- this formulation is said as wound cleanser. Most of the ingredients like triphala,[35] khadira, daruharidra, nyagrodhadi group nimb, haridra, daruharidra, madhuka are the ingredients of jatyadi taila /ghrita which is well known formulation in managment of chronic wound for shodhan and ropan of wounds. [36],[37],[38],[39],[40],[41],[42]
- The drugs which are helpful for healing of fresh and infected or chronic wounds are mentioned in the text. Among these drugs following drugs are having some research studies carried out for their healing effect.Decoction of Panchavalkal (nyagrodha, udumbara, asvattha, parish plaksha), karavira (Nerium indicum Mill.), arka (Calotropis procera R. Br.)[43] and kutaja (Holarrhena antidysentrica Linn.) are wound healing. Candana (Santalum album Linn.), daruharidra bark, meda (Polygonatum airrhifolium Royle), mahameda (Polygonatum airrhifolium Royle), murva (Marsdenia tenacissima W. & A.), lajjalu (Mimosa pudica Linn.) and madhuyasti[44]- this formulation is wound healer. Prapaundarika, jivanti, gojihva (Onosma bracteatum Wall.), dhataki, bala and sesamum should be applied as paste with ghee for wound healing. Kampillaka (Mallotus philippinensis Muell Arg), vidanga (Embelia ribes Burm), kutaja, triphala, bala, patola (Trichosanthes dioica Roxb.), nimba, musta (Cyperus rotundus Linn.), priyangu, khadira, dhataki, sarja, ela (Elleteria cardamomum Maton.), aguru (Aquilaria agallocha Roxb.) and candana are pounded together and used for cooking oil. This oil is used as ulcer healing agent. Similarly, oil prepared with equal quantity of prapaundarika, mahuka, kakoli (Roscoca procera Wall.), ksirakakoli (Roscoca procera Wall.), chandana and rakta chandana (Pterocarpus santalinus Linn.)[45] is an excellent ulcer healing agent. Oil cooked with durva juice or kampillaka or paste of daruharidra bark is an important ulcer healer.[46],[47],[48] By the above method ghrita should be prepared and used for healing, ulcers predominant in rakta and pitta.
- The physician conversant with dose, time and agni (heat) may apply alkali in cases amenable to surgical operations.[49],[50],[51],[52]
- By dusting the wound with the powders of barks of kakubha (Termalia arjuna),[53] udumbara,[54] ashvattha, lodhra (Symplocos racemosa Roxb), jambu (Eugenia jambolana Lam) and katphala (Myrica esculenta Buch-Ham) they heals the skin quickly. Manashila (Realgar), manjistha,[55],[56] lac, haridra and daruharidra used as paste with ghee and honey is an excellent cleanser of skin.
Potential areas /Scope for research
The ingredients like bala (Sida cordifolia Linn.), kusa (Desmostachya bipinnata Stapf.), badara (Zizyphus jujube Lam.), trivrit (Operculina turpethum Linn.), karavira (Nerium indicum Mill.), kutaja (Holarrhena antidysentrica Linn.), meda (Polygonatum airrhifolium Royle), mahameda (Polygonatum airrhifolium Royle), murva (Marsdenia tenacissima W. & A.), lajjalu (Mimosa pudica Linn.), gojihva (Onosma bracteatum Wall.), dhataki, ela (Elleteria cardamomum Maton.), aguru (Aquilaria agallocha Roxb.), kakoli (Roscoca procera Wall.), ksirakakoli (Roscoca procera Wall.) are mentioned for wound healing so there is a scope to find out their clinical wound healing effect.
Charak mentioned some formulations for shodhan (cleansing) and ropan (healing) in this chapter. Along with single drug these formulations need to be further studied for their scientific validation.
Shodhana (Cleansing) formulations
- Decoctions of triphala, khadira (Acasia catechu Willd), daruharidra (Berberis aristata DC), nyagrodhadi group, bala (Sida cordifolia Linn.), kusa (Desmostachya bipinnata Stapf.), leaves of nimb (Azadirachta indica A. Juss) and badara (Zizyphus jujube Lam.) are regarded as cleansing drugs.
- Tila paste, salt, haridra (Curcuma longa Linn.), daruharidra (Berberis aristata DC), trivrit (Operculina turpethum Linn.) ghrita, madhuka, nimba leaves.
- Manahsila (Realgar), manjistha, lac, haridra and daruharidra used as paste with ghee and honey
- Ropan (healing) formulations:
- Decoction of nyagrodha, udumbara, asvattha, kadamba, plaksha, vetasa, karavira (Nerium indicum Mill.), arka (Calotropis procera R. Br.) and kutaja (Holarrhena antidysentrica Linn.) are wound healing. Candana (Santalum album Linn.), lotus stamens, daruharidra bark, blue water lily, meda (Polygonatum airrhifolium Royle), mahameda (Polygonatum airrhifolium Royle), murva (Marsdenia tenacissima W. & A.), lajjalu (Mimosa pudica Linn.) and madhuyasti-
- Pase of ghee prepared with Prapaundarika, jivanti, gojihva (Onosma bracteatum Wall.), dhataki, bala and sesamum
- Oil of Kampillaka (Mallotus philippinensis Muell Arg), vidanga (Embelia ribes Burm), kutaja, triphala, bala, patola (Trichosanthes dioica Roxb.), nimba, musta (Cyperus rotundus Linn.), priyangu, khadira, dhataki, sarja, ela (Elleteria cardamomum Maton.), aguru (Aquilaria agallocha Roxb.) and candana
- Oil prepared with equal quantity of prapaundarika, mahuka, kakoli (Roscoca procera Wall.), ksirakakoli (Roscoca procera Wall.), chandana and rakta chandana (Pterocarpus santalinus Linn.)
- Oil cooked with durva juice or kampillaka or paste of daruharidra bark.
- Powders of barks of kakubha (Termalia arjuna), udumbara, asvattha, lodhra (Symplocos racemosa Roxb), jambu (Eugenia jambolana Lam) and katphala (Myrica esculenta Buch-Ham).
Remedies for post healing complications
- The paste prepared by bhasmas of iron, kasisa and triphala (haritaki,vibhitaki and amalaki) flowers provides blackness in the newly formed skin quickly.
- Kaliyaka (Jateorhiza palmata Miers), nata /tagara (Valeriana wallichii DC), mango seeds, nagakesara, iron and triphala powder mixed with cow-dung juice make an excellent paste for reviving normal colour in skin.
- Roots of dhyamaka, asvattha and nicula (Barringtonia acutangula Linn), lac, gairic(red-ochre), nagakesara and kasisa-These restores the natural colour of the skin.
- Lodhra, leafbuds of nyagrodha, khadira, triphala and ghrita - this combination used as paste provides looseness and softness in wounds.
The role of diet is very important in wounded patients which can be considered for further research as Charak mentioned that wounded patients should abstain from salt, sour, pungent, hot, burning and heavy food and drinks and also sexual intercourse.
Send us your suggestions and feedback on this page.
References
- ↑ Sushruta. Chikitsa Sthana, Cha.1 Dwivraneeya Chikitsitam Adhyaya verse 134. In: Kaviraja Ambikadutta Shastri Editors. Sushruta Samhita. reprint ed. Varanasi: Chaukhambha Sanskrit Sansthan;2013. pp 16.
- ↑ Sushruta. Chikitsa Sthana, Cha.2 Sadyovrana Chikitsitam Adhyaya verse 12. In: Kaviraja Ambikadutta Shastri Editors. Sushruta Samhita. reprint ed. Varanasi: Chaukhambha Sanskrit Sansthan;2013. pp 16.
- ↑ Vagbhata. Uttara Sthana, Cha.26 Sadyovranapratishedha Adhyaya verse 13. In: Kaviraj Atrideva Gupta, Editors. Ashtanga Hridayam. Reprint ed. Varanasi: Chaukhambha Sanskrit Sansthan;2005.pp 26
- ↑ Sushruta. Chikitsa Sthana, Cha.1 Dwivraniya Chikitsitam Adhyaya verse 27-18. In: Jadavaji Trikamji Aacharya, Editors. Sushruta Samhita. 8th ed. Varanasi: Chaukhambha Orientalia;2005. p.1.
- ↑ 5.0 5.1 Sushruta. Chikitsa Sthana, Cha.1 Dwivraneeya Chikitsitam Adhyaya verse 8. In: Jadavaji Trikamji Aacharya, Editors. Sushruta Samhita. 8th ed. Varanasi: Chaukhambha Orientalia;2005. p.1.
- ↑ Bhela, Chikitsa sthana, Chap.27, Verse 14-15 . In:K. H. Krishnamurthy,Prof. P.V. Sharma Editors, reprint edition, Varanasi; Chaukhambha Visvabharati, 2008, pp 468.
- ↑ Sushruta. Chikitsa Sthana, Cha.3 Bhagnachikisitam Adhyaya verse 18-19. In: Kaviraja Ambikadutta Shastri Aacharya, Editors. Sushruta Samhita. Reprint ed. Varanasi: Chaukhambha Sanskrit Sansthan;2013. pp 28.
- ↑ Sushruta. Chikitsa Sthana, Cha.3 Bhagnachikisitam Adhyaya verse 4-5. In: Kaviraja Ambikadutta Shastri Aacharya, Editors. Sushruta Samhita. Reprint ed. Varanasi: Chaukhambha Sanskrit Sansthan;2013. pp 28.
- ↑ Sushruta. Sutra Sthana, Cha.25 Ashtavidashastrakarmeeya Adhyaya verse 10. In: Jadavaji Trikamji Aacharya, Editors. Sushruta Samhita. 8th ed. Varanasi: Chaukhambha Orientalia;2005. p.1.
- ↑ Sushruta. Sutra Sthana, Cha.18 Vranalepanabandhavidhi Adhyaya verse 17. In: Kaviraja Ambikadutta Shastri, Editors. Sushruta Samhita. Reprint ed. Varanasi: Chaukhambha Sanskrit Sansthan;2013. pp 98
- ↑ Vagbhata. Sutra Sthana, Cha.29 Shastrakarmavidhi Adhyaya verse 59-60. In: Kaviraj Atrideva Gupta, Editors. Ashtanga Hridayam. reprint ed. Varanasi:Chaukhambha Sanskrit Sansthan,2005.p.4.pp 161
- ↑ Vagbhata. Sutra Sthana, Cha.6 Annaswarupavijnaneeyam Adhyaya verse 143. In: Kaviraj Atrideva Gupta, Editors. Ashtanga Hridayam. Reprint ed. Varanasi: Chaukhambha Sanskrit Sansthan;2005 pp 64.
- ↑ Sushruta. Sutra Sthana, Cha.14 Shonitavarnaneeya Adhyaya verse 40. In: Kaviraja Ambikadutta Shastri, Editors. Sushruta Samhita. Reprint ed. Varanasi: Chaukhambha Sanskrit Sansthan;2013. pp 72
- ↑ Sushruta. Sutra Sthana, Cha.5 Agropaharaneeya Adhyaya verse 17. In: Kaviraja Ambikadutta Shastri, Editors. Sushruta Samhita. Reprint ed. Varanasi:Chaukhambha Sanskrit Sansthan ;2013. pp 24.
- ↑ Vagbhata. Uttara Sthana, Cha.25 Vranapratishedha Adhyaya verse 45. In: Kaviraj Atrideva Gupta,Editors. Ashtanga Hridayam. Reprint ed. Varanasi: Chaukhambha Sanskrit Sansthan;2005.pp 542.
- ↑ Dwivedi SP, Shukla DV. Role of Jalaukavacharana (leech therapy) in the management of ankle sprain: a pilot study. International journal of Ayurveda & Alternative Medicine. 2014; 2 (4): 92-95.
- ↑ Pandey BB, Kumar A, Singh N, Bhatia. Efficacy of Jalaukavcharana (Leech Application) in Ischemic Ulcer with Pre-Gangrenous Changes - A Case Report, Journal of Ayurveda 2012 Jul-Sep ; 4 (3) :103-107.
- ↑ Lad M, Bandgar S. Management of non healing wound with nyagrodhadi kwatha and jatyadi ghruta (classical ayurvedic preparations). Global Journal of Research on Medicinal Plants & Indigenous Medicine (GJRMI). 2012; 1 (7): 301-308.
- ↑ Meena RK, Dudhamal T, Gupta SK, Mahanta V. Wound healing potential of Pañcavalkala formulations in a postfistulectomy wound. Ancient Sci Life (ASL) 2015;35 (2):118-21
- ↑ Bhat KS, Vishwesh BN, Sahu M, Shukla VK. A clinical study on the efficacy of panchavalkala cream in vrana shodhana w.s.r to its action on microbial load and wound infection. AYU. 2014;35(2):135-140
- ↑ K. Shobha Bhat, M. Sahu, V.K. Shukla. Efficacy of pancavalkala cream in the management of chronic non-healing wounds, Aryavaidyan 2013 May-July ; (26) :224-228
- ↑ Khadkutkar DK, Prof. Kanthi Veena. Therapeutic uses of Panchvalkala in different forms-a review. Ayurlog; National Journal of Research in Ayurveda Science. 2014; 2(1): 1-5
- ↑ Khadkutkar DK, Prof. Kanthi Veena G. A Brief Review of Research Studies Conducted on Panchavalkal. Indian Journal of Ancient Medicine and Yoga. 2015;8(2): 87-94
- ↑ Khadkutkar DK, Kanthi VG, Dudhamal TS. Antimicrobial activity of Panchavalkal powder and ointment. International Journal of Medicinal Plants and Natural Products (IJMPNP). 2015; 1(3): 9-15
- ↑ Dudhamal TS, Gupta SK, Bhuyan C. Role of honey (madhu) in the management of wounds (dushta vrana). International Journal of Ayurveda Research. 2010; 1 (4): 271-273
- ↑ Vijayakumari K, Nishteswar K. Wound Healing Activity of Honey: A Pilot Study. AYU. 2013; 33 (3): 374-377.
- ↑ Gupta S, Bhat SS, Jaykrishna N. A clinical study to evaluate efficacy of nimbaadya taila in the management of dusta vrana (chronic ulcer). International Journal of Research in Ayurveda and Pharmacy.2012; 3(6):862-865
- ↑ Jayasingh BK, Tewari PV. Clinical management of vicharchika with nimbadi yoga. Journal of Research in Ayurveda and Siddha. 2003; 24(1-2): 33-41
- ↑ Singh A, Singh AK, Narayan G, Singh TB, Shukla VK. Effect of Neem Oil and Haridra on Non-Healing Wounds. AYU. 2014;35 (4) : 398-403
- ↑ Singh AK, Srivastava PK, Shukla VK. Evaluation of nimba taila and manjistha churna in non healing ulcer. International Research Journal of Pharmacy. 2011; 2(5):201-210.
- ↑ Ballal V, Mamatha, Jain CM. A clinical study on efficacy of kumarimajja and haridra on episiotomy wound. Journal of Ayurveda. 2010; 4(2): 18-26
- ↑ Kundu S, Biswas TK, Das P, Kumar S, De DK. Turmeric (Curcuma longa) rhizome paste and honey show similar Wound healing potential: a preclinical study in rabbits, The international Journal of Lower Extremity Wounds 2005 Dec ; 4(4):205-13
- ↑ Mehra KS, Mikuni I, Gupta U, Gode KD. Curcuma longa (Linn) drops in corneal wound healing, The Tokai Journal of Experimental and Clinical Medicine 1984 Mar ; 9 (1) :27-31
- ↑ Saravanakumar T, Venkatasubramanian P, Vasanthi NS, Manonmani E. Antimicrobial potential of Daruharidra (Berberis aristata DC) against the pathogens causing eye infection. Int J Green Pharm 2014;8:153-7
- ↑ Senthil KM, Kirubanandan S, Sripriya R, Sehgal PK. Triphala incorporated collagen sponge--a smart biomaterial for infected dermal wound healing, The Journal of Surgical Research 2010 158(1):162-70
- ↑ Kulkarni YS, Emmi SV, Dongargaon TN, Wali AA. Wound healing effect of Vimlapanakarma with Jatyadi tailam in diabetic foot, Ancient Science of Life 2015;34(3):171-174
- ↑ Dudhamal TS, Bhuyan C, Baghel MS. Wound healing effect of Jatyadi Taila in the cases of chronic fissure-in-ano treated with Ksharasutra. AYU International Research Journal of Ayurved 2013; 34/5 (Suppl1) OA01:30.p-22.
- ↑ Vijakumar B, Prasanna N. Rao PN, Hemantkumar P. A comparative study of kaseesadi avachurnana and jatyadi ghrita application in the management of dushta vrana. International Journal of Research in Ayurveda and Pharmacy. 2012; 3(6):852-858
- ↑ Baslingappa Rajeshwari KPN, Aravattii S, Murthy BN, Shringi MK.Comparative clinical study of Jatyadi varti and Aragwadadi varti in the management of nadi vrana (pilonidal sinus). International Research Journal of Pharmacy. 2012;3(3):135-138
- ↑ Lad M, Bandgar S. Management of non healing wound with Nyagrodhadi kwatha and Jatyadi ghruta (classical ayurvedic preparations). Global Journal of Research on Medicinal Plants & Indigenous Medicine (GJRMI). 2012; 1 (7): 301-308
- ↑ Pal R, Apaturkar N, Pimpalkar P, Raut S, Lakhapati AM. Role of Jatyadi tailam vrana basti in the management of post operated haemorrhoidectomy. e-Journal Rasamruta. 2013; 5 (38): 1-5
- ↑ Shailajan S, Menon S, Pednekar S, Singh A. Wound healing efficacy of Jatyadi Taila: in vivo evaluation in rat using excision Wound model, Journal of Ethnopharmacology 2011 Oct 31; 138 (1) :99-104
- ↑ Deshmukh PT, Fernandes J, Atul A, Toppo E. Wound healing activity of Calotropis gigantea root bark in rats, Journal of Ethnopharmacology 2009; 125(1):178-81
- ↑ Dwivedi Ap, Rahtod AS, Dhariya SA. A clinical study to evaluate the antiseptic and bactericidal effect of yashtimadhu ghrita in non infected surgical wounds. International Journal of Applied Ayurved Research. 2015;2(3):248-252
- ↑ Biswas TK, Maity LN, Mukherjee B. Wound healing potential of Pterocarpus santalinus linn: a pharmacological evaluation, The international Journal of Lower Extremity Wounds 2004 Sep ; 3 (3) :143-50
- ↑ Pankhaniya LJ, Sharma PP, Manjusha R. A comparative study of Durvadi taila and povidone iodine in the management of vrana. AYU. 2009;30(4): 459-462
- ↑ Jadhav NM, Auti SS, Sreeja S, Mourya OPS. Management of corneal erosions due to chemical burn by Durvadi ghritam: a case study. Ayurpharm - International Journal of Ayurveda and Allied Sciences. 2012; 1 (4) : 73-76
- ↑ Dhiman K, Parmar M, Dhiman KS. Kampillakadi Ghrita In Garbhashaya Greeva Gata Vrana (Cervical Erosion). International Journal of Research in Ayurveda and Pharmacy. 2012; 3 (2):203-209
- ↑ Wani P, Pathak A, Hemanthakumar P. Effect of Apamarga pratisaraeeya kshara in the management of nadivrana (pilonidal sinus) – a case report. International Ayurvedic Medical Journal. 2013; 1 (4) : 1-2.
- ↑ Shekokar AV, Borkar KM. Innovation of Ksharaplota (medicated gauze) in the management of vrana (ulcer). International Journal of Ayurveda and Pharma Research. 2013; 1 (2):10-16.
- ↑ Gupta S, Gupta SJ, Singh SK. Role of Palashkshara (butea monosperma) in the management of dusta vrana (chronic ulcers) with special reference to infected wound. International Journal of Ayurveda and Pharma Research. 2014; 2 (3): 86-93
- ↑ Apaturkar N, Pimpalkar P, Pal R, Raut S, Lakhapati AM. Role of Apamarga Kshara with apamarga kshara tailam on dushtavrana with reference to infected wound – a case report. e-Journal Rasamruta. 2013; 5 (26): 1- 8.
- ↑ Narayana A, Swamy RK . A medico-historical review of Arjuna (Terminalia arjuna, w. & a.). Bulletin of the Indian Institute of History of Medicine. 1998; 26(1-2): 1-10
- ↑ Vinaya Kumar, P.V. Tiwari. Post-Cautery Effect of Udumbar Ointment on Cervical Erosion, Ancient Science of Life 1993 July ; 13 (1-2) :97-101
- ↑ Baria J, Gupta SK, Bhuyan C. Clinical Study of Manjishthadi Ghrita in Vrana Ropana. AYU. 2011; 32 (1): 95-99.
- ↑ Singh AK, Srivastava PK, Shukla VK. Evaluation of Nimba taila and Manjistha churna in non healing ulcer. International Research Journal of Pharmacy. 2011; 2(5):201-210